Introduction
- Leptospira species are thin, spiral-shaped bacteria belonging to the family Leptospiraceae.
- Among them, Leptospira interrogans is the most important pathogenic species responsible for leptospirosis.
- Leptospirosis is a zoonotic disease with a wide spectrum of clinical manifestations, ranging from mild flu-like illness to severe, life-threatening disease.
- The infection is commonly associated with exposure to water or soil contaminated with animal urine.
- Understanding the microbiological characteristics, pathogenic mechanisms, and laboratory diagnosis is essential for early detection and effective management.
- Public health measures, education, and preventive strategies play a vital role in controlling leptospirosis, especially in endemic regions.
General Character
Genus: Leptospira
Taxonomic Classification
-
Genus: Leptospira
-
Family: Leptospiraceae
Medically Important Species
-
Leptospira interrogans – Causes leptospirosis
-
Other species:
-
Several pathogenic and saprophytic species exist
-
They differ in pathogenic potential, host preference, and environmental adaptability
-
Morphological Characteristics
Gram Staining
-
Leptospira species are Gram-negative
-
Poorly visualized by routine Gram staining due to:
-
Extremely thin cell wall
-
Delicate structure
-
-
Best demonstrated by:
-
Dark-field microscopy
-
Phase-contrast microscopy
-
Silver impregnation techniques
-
Shape and Arrangement
-
Shape:
-
Slender spirochetes with a characteristic helical structure
-
Ends are often hooked, giving a question-mark appearance
-
-
Arrangement:
-
Usually present as single organisms
-
Occasionally seen in pairs
-
Oxygen Requirement
-
Leptospira species are microaerophilic
-
Require low oxygen tension for optimal growth
-
Excess oxygen inhibits growth
Morphology
Size
-
Length: 6–20 µm
-
Diameter: ~0.1 µm
-
Among the thinnest bacteria, making visualization difficult
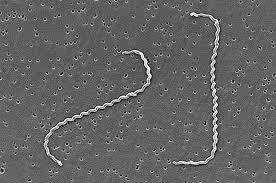
Shape
-
Spirochete with tightly coiled helical structure
-
Characteristic hooked ends, giving a question-mark or fish-hook appearance
-
Coils are fine and closely spaced
Arrangement
-
Usually seen as single, free-living organisms
-
Occasionally observed in pairs
-
Do not form chains or clusters
Cell Structure
-
Gram-negative, but poorly stained with routine Gram stain
-
Cell envelope consists of:
-
Outer membrane
-
Thin peptidoglycan layer
-
Cytoplasmic membrane
-
-
No capsule and no spore formation
Motility
-
Actively motile
-
Exhibits rapid rotatory and flexing movements
-
Motility is due to periplasmic flagella (axial filaments) located between the cell wall and outer membrane
-
Motility helps in:
-
Penetration of mucous membranes
-
Tissue invasion
-
Staining Characteristics
-
Not easily visualized by:
-
Gram stain
-
Routine stains
-
-
Best demonstrated by:
-
Dark-field microscopy
-
Phase-contrast microscopy
-
Silver impregnation stains (Warthin–Starry)
-
Immunofluorescence techniques
-
Special Morphological Features
-
Extremely fragile organism
-
Survives poorly in dry conditions
-
Maintains viability longer in moist environments
Cultural Characteristics
Growth on Artificial Media
-
Leptospira species can be cultured, unlike Treponema
-
Require special enriched media
-
Commonly used media:
-
EMJH medium (Ellinghausen–McCullough–Johnson–Harris) – most commonly used
-
Fletcher’s medium
-
Stuart’s medium
-
Oxygen Requirement
-
Microaerophilic
-
Require low oxygen tension for optimal growth
-
Excess oxygen inhibits growth
Temperature Requirement
-
Optimum growth temperature: 28–30°C
-
Do not grow well at 37°C
-
Growth is better at room temperature than body temperature
pH Requirement
-
Optimal pH: 7.2–7.6
-
Slightly alkaline environment favors growth
Growth Characteristics
-
Growth is slow
-
Generation time is long
-
Visible growth appears after 1–4 weeks
-
Growth appears as:
-
Subsurface ring (Dinger’s ring) in semi-solid media
-
Uniform turbidity in liquid media
-
Colony Morphology
-
No discrete colonies on solid media
-
Growth observed only in liquid or semi-solid media
-
Colonies are usually examined using dark-field microscopy
Sensitivity to Environment
-
Sensitive to:
-
Drying
-
Heat
-
Disinfectants
-
-
Survives longer in:
-
Moist soil
-
Stagnant water
-
Laboratory Significance
-
Culture is mainly used for:
-
Research
-
Epidemiological studies
-
-
Not routinely used for diagnosis due to:
-
Slow growth
-
Risk of laboratory infection
-
Biochemical Reactions
Catalase Test
-
Result: Positive
-
Indicates the presence of catalase enzyme
-
Helps the organism survive oxidative stress
Oxidase Test
-
Result: Positive
-
Presence of cytochrome oxidase enzyme
-
Supports their aerobic–microaerophilic metabolism
Carbohydrate Utilization
-
Do not ferment carbohydrates
-
No acid or gas production in routine carbohydrate fermentation tests
-
Energy is derived from:
-
Long-chain fatty acids
-
Amino acids
-
Metabolic Characteristics
-
Possess an oxidative metabolism
-
Depend on fatty acid oxidation rather than glucose metabolism
-
Require enriched media supplying fatty acids for growth
Pathogenicity
Reservoirs of Infection
-
Rodents (especially rats) – most important reservoir
-
Domestic animals:
-
Cattle
-
Pigs
-
Dogs
-
-
Organisms are excreted in urine of infected animals
Mode of Transmission
-
Humans are infected through:
-
Abraded skin
-
Intact mucous membranes (conjunctiva, oral mucosa)
-
-
Exposure to:
-
Water or soil contaminated with animal urine
-
-
Occupational and recreational exposure (farmers, sewage workers, flood exposure)
Portal of Entry
-
Cuts and abrasions on skin
-
Mucous membranes of eyes, nose, and mouth
Virulence Factors and Pathogenic Mechanisms
1. Motility
-
Active motility due to periplasmic flagella
-
Enables penetration of:
-
Skin
-
Mucous membranes
-
Tissues
-
2. Adhesion
-
Surface proteins facilitate attachment to host cells
-
Promotes colonization of tissues, especially kidneys
3. Endotoxin-Like Activity
-
Lipopolysaccharide (LPS)-like components
-
Induces:
-
Fever
-
Inflammation
-
Vascular damage
-
4. Immune Evasion
-
Ability to survive in blood and tissues
-
Evades host immune response leading to systemic spread
5. Vascular Damage
-
Causes capillary endothelial damage
-
Results in:
-
Hemorrhage
-
Jaundice
-
Renal dysfunction
-
Pathogenesis of Leptospirosis
Phase 1: Septicemic Phase
-
Organisms present in blood and CSF
-
Sudden onset of:
-
High fever
-
Headache
-
Severe myalgia
-
Conjunctival suffusion
-
Phase 2: Immune Phase
-
Appearance of antibodies
-
Organisms disappear from blood
-
Persist in:
-
Kidneys (excreted in urine)
-
-
Leads to:
-
Meningitis
-
Renal and hepatic involvement
-
Clinical Forms of Leptospirosis
Anicteric Leptospirosis
-
Mild, self-limiting disease
-
Fever, headache, muscle pain
Icteric Leptospirosis (Weil’s Disease)
-
Severe form
-
Features:
-
Jaundice
-
Acute renal failure
-
Hemorrhagic manifestations
-
-
High mortality if untreated
Host Immune Response
-
Both humoral and cell-mediated immunity involved
-
Antibodies help clear organisms from blood
-
Persistence in kidneys leads to urinary shedding
Laboratory Diagnosis
1. Specimen Collection
-
Blood – during the early (septicemic) phase (1st week)
-
Cerebrospinal fluid (CSF) – early phase in suspected meningitis
-
Urine – during the immune phase (after 1st week)
-
Serum – for serological tests
2. Direct Demonstration of the Organism
a. Dark-Field Microscopy
-
Specimens: Blood, CSF, urine
-
Shows:
-
Thin, motile spirochetes with hooked ends
-
-
Limitations:
-
Low sensitivity
-
Requires experienced observer
-
Artifacts may cause false interpretation
-
b. Phase-Contrast Microscopy
-
Alternative to dark-field microscopy
-
Better visualization of live organisms
3. Culture
-
Leptospira can be cultured, but growth is slow
-
Media used:
-
EMJH medium (most commonly used)
-
Fletcher’s medium
-
-
Optimal conditions:
-
Temperature: 28–30°C
-
Microaerophilic environment
-
-
Growth appears after 1–4 weeks
-
Not routinely used due to:
-
Slow growth
-
Risk of laboratory-acquired infection
-
4. Serological Tests
a. Microscopic Agglutination Test (MAT)
-
Gold standard test
-
Detects serovar-specific antibodies
-
Useful for:
-
Confirming diagnosis
-
Epidemiological studies
-
-
Requires paired sera showing rising antibody titer
b. ELISA
-
Detects IgM antibodies
-
Useful for early diagnosis
-
More sensitive and rapid than MAT
c. Other Serological Tests
-
Latex agglutination
-
Rapid card tests
(Used for screening in endemic areas)
5. Molecular Methods
Polymerase Chain Reaction (PCR)
-
Detects Leptospira DNA
-
Useful in:
-
Early phase before antibodies appear
-
Severe cases
-
-
High sensitivity and specificity
-
Limited availability
6. Supportive Laboratory Findings
-
Raised serum bilirubin
-
Elevated liver enzymes
-
Increased creatinine and urea
-
Thrombocytopenia
Antibiotic Resistance
Antibiotic Susceptibility Pattern
-
Penicillin G – drug of choice for severe leptospirosis
-
Doxycycline – effective in mild disease and for prophylaxis
-
Ceftriaxone / Cefotaxime – effective alternatives, especially in severe cases
-
Azithromycin – useful alternative in mild cases
Resistance Profile
-
No widespread or stable resistance reported in Leptospira species
-
Treatment failures are usually due to:
-
Delay in diagnosis
-
Late initiation of therapy
-
Severe organ damage rather than true resistance
-
Mechanisms Limiting Resistance Development
-
Limited horizontal gene transfer
-
Absence of plasmid-mediated resistance
-
Slow growth rate and specialized metabolism
-
Obligate dependence on specific environmental conditions
Laboratory Detection of Resistance
-
Routine antibiotic susceptibility testing is not performed
-
Culture-based sensitivity testing is difficult due to:
-
Slow growth
-
Special media requirements
-
-
Resistance data mainly derived from:
-
Clinical response
-
Experimental and surveillance studies
-
Prevention
1. Control of Reservoirs
-
Rodent control is the most important preventive measure
-
Proper disposal of garbage to reduce rat population
-
Control of infection in domestic animals through veterinary care
2. Environmental Measures
-
Avoid contact with stagnant or flood water, especially in endemic areas
-
Improve sanitation and drainage systems
-
Safe disposal of animal waste
3. Personal Protective Measures
-
Use of protective clothing (boots, gloves) by:
-
Farmers
-
Sewage workers
-
Veterinarians
-
-
Covering cuts and abrasions while working in wet environments
4. Chemoprophylaxis
-
Doxycycline (weekly) recommended for:
-
High-risk individuals
-
During outbreaks
-
Occupational exposure
-
5. Health Education and Awareness
-
Educating communities about:
-
Modes of transmission
-
Risk factors
-
Early symptoms
-
-
Promotion of hygienic practices
6. Occupational Safety
-
Safety measures for:
-
Agricultural workers
-
Sewer and sanitation workers
-
-
Use of personal protective equipment (PPE)
7. Public Health Measures
-
Surveillance and early detection of cases
-
Prompt treatment to reduce complications
-
Reporting of cases during outbreaks
8. Vaccination
-
No widely used human vaccine available
-
Animal vaccination is used in some countries to reduce transmission
MCQs
1. Leptospira belongs to which family?
A. Spirochaetaceae
B. Leptospiraceae
C. Enterobacteriaceae
D. Mycobacteriaceae
✅ Answer: B
2. The causative agent of leptospirosis is:
A. Leptospira biflexa
B. Leptospira interrogans
C. Treponema pallidum
D. Borrelia recurrentis
✅ Answer: B
3. Leptospira species are best described as:
A. Curved bacilli
B. Straight rods
C. Spiral-shaped spirochetes
D. Cocci
✅ Answer: C
4. Characteristic morphological feature of Leptospira is:
A. Thick capsule
B. Flagella at poles
C. Hooked ends
D. Spores
✅ Answer: C
5. Leptospira is poorly visualized by Gram stain because:
A. No cell wall
B. Acid-fast nature
C. Extremely thin structure
D. Capsule presence
✅ Answer: C
6. Best method to visualize live Leptospira organisms:
A. Gram stain
B. Ziehl–Neelsen stain
C. Dark-field microscopy
D. India ink
✅ Answer: C
7. Motility of Leptospira is due to:
A. Polar flagella
B. Pili
C. Axial filaments
D. Cilia
✅ Answer: C
8. Oxygen requirement of Leptospira species:
A. Obligate anaerobe
B. Facultative anaerobe
C. Microaerophilic
D. Obligate aerobe
✅ Answer: C
9. Culture medium commonly used for Leptospira:
A. Blood agar
B. MacConkey agar
C. EMJH medium
D. Lowenstein–Jensen medium
✅ Answer: C
10. Optimal temperature for growth of Leptospira:
A. 37°C
B. 25°C
C. 28–30°C
D. 42°C
✅ Answer: C
11. Growth of Leptospira on culture media is:
A. Rapid
B. Moderate
C. Slow
D. Immediate
✅ Answer: C
12. Typical growth pattern of Leptospira in semi-solid media:
A. Surface pellicle
B. Bottom sediment
C. Dinger’s ring
D. Hemolysis
✅ Answer: C
13. Catalase test for Leptospira is:
A. Negative
B. Weakly positive
C. Positive
D. Variable
✅ Answer: C
14. Oxidase test for Leptospira is:
A. Negative
B. Positive
C. Variable
D. Not applicable
✅ Answer: B
15. Leptospira derives energy mainly from:
A. Glucose
B. Lactose
C. Fatty acids
D. Starch
✅ Answer: C
16. Carbohydrate fermentation by Leptospira:
A. Positive
B. Weakly positive
C. Variable
D. Negative
✅ Answer: D
17. Main reservoir of Leptospira interrogans is:
A. Birds
B. Dogs
C. Rodents
D. Humans
✅ Answer: C
18. Mode of transmission of leptospirosis:
A. Airborne
B. Sexual contact
C. Exposure to contaminated water
D. Vector-borne
✅ Answer: C
19. Portal of entry of Leptospira into humans:
A. Intact skin only
B. Abraded skin and mucous membranes
C. Respiratory tract
D. Gastrointestinal tract
✅ Answer: B
20. Leptospirosis is classified as:
A. Nosocomial infection
B. Opportunistic infection
C. Zoonotic disease
D. Opportunistic fungal infection
✅ Answer: C
21. Early phase of leptospirosis is known as:
A. Immune phase
B. Latent phase
C. Septicemic phase
D. Chronic phase
✅ Answer: C
22. Organisms are present in blood during:
A. Immune phase
B. Septicemic phase
C. Convalescent phase
D. Late phase only
✅ Answer: B
23. Later phase of leptospirosis is called:
A. Septicemic phase
B. Incubation phase
C. Immune phase
D. Carrier phase
✅ Answer: C
24. Characteristic clinical feature of leptospirosis:
A. Koplik spots
B. Conjunctival suffusion
C. Strawberry tongue
D. Eschar
✅ Answer: B
25. Severe leptospirosis with jaundice is called:
A. Dengue shock syndrome
B. Weil’s disease
C. Typhoid fever
D. Brucellosis
✅ Answer: B
26. Weil’s disease is characterized by:
A. Rash and lymphadenopathy
B. Jaundice and renal failure
C. Pneumonia
D. Diarrhea
✅ Answer: B
27. Organ most commonly colonized by Leptospira:
A. Liver
B. Spleen
C. Kidney
D. Lung
✅ Answer: C
28. Urinary shedding of Leptospira occurs during:
A. Septicemic phase
B. Immune phase
C. Incubation period
D. Primary phase
✅ Answer: B
29. Gold standard serological test for leptospirosis:
A. ELISA
B. Weil–Felix test
C. MAT
D. VDRL
✅ Answer: C
30. MAT stands for:
A. Microbial Antibody Test
B. Microscopic Agglutination Test
C. Molecular Antigen Test
D. Macroscopic Agglutination Test
✅ Answer: B
31. ELISA in leptospirosis commonly detects:
A. IgG
B. IgA
C. IgM
D. IgE
✅ Answer: C
32. Best specimen during first week of illness:
A. Urine
B. Blood
C. Stool
D. Saliva
✅ Answer: B
33. Best specimen after first week of illness:
A. Blood
B. CSF
C. Urine
D. Sputum
✅ Answer: C
34. PCR is useful in leptospirosis because:
A. It is cheap
B. Detects antibodies
C. Detects DNA early
D. Used only in late disease
✅ Answer: C
35. Drug of choice for severe leptospirosis:
A. Doxycycline
B. Azithromycin
C. Penicillin G
D. Ciprofloxacin
✅ Answer: C
36. Drug used for prophylaxis in leptospirosis:
A. Penicillin
B. Rifampicin
C. Doxycycline
D. Amoxicillin
✅ Answer: C
37. Antibiotic resistance in Leptospira is:
A. Common
B. Increasing
C. Rare
D. Universal
✅ Answer: C
38. Leptospira biflexa is:
A. Highly pathogenic
B. Mildly pathogenic
C. Saprophytic
D. Opportunistic
✅ Answer: C
39. Occupational risk group for leptospirosis includes:
A. Teachers
B. Farmers
C. Office workers
D. Shopkeepers
✅ Answer: B
40. Seasonal outbreaks of leptospirosis commonly occur during:
A. Winter
B. Summer
C. Monsoon
D. Autumn
✅ Answer: C
41. Prevention of leptospirosis mainly includes:
A. Vaccination
B. Vector control
C. Rodent control
D. Isolation of patients
✅ Answer: C
42. Human vaccine for leptospirosis is:
A. Widely available
B. Partially effective
C. Under trial only
D. Not widely used
✅ Answer: D
43. Leptospira survives best in:
A. Dry soil
B. Acidic environment
C. Moist environment
D. High temperature
✅ Answer: C
44. Leptospirosis is commonly associated with:
A. Desert regions
B. Floods
C. Snowfall
D. High altitude
✅ Answer: B
45. Incubation period of leptospirosis is usually:
A. 1–2 days
B. 2–5 days
C. 7–14 days
D. 1–2 months
✅ Answer: C
46. Most sensitive test in early leptospirosis:
A. MAT
B. ELISA
C. PCR
D. Culture
✅ Answer: C
47. Non-pathogenic Leptospira species are usually:
A. Found in humans
B. Found in soil and water
C. Found in blood
D. Hospital-acquired
✅ Answer: B
48. Main public health importance of leptospirosis:
A. Person-to-person spread
B. High mortality in children
C. Zoonotic and environmental spread
D. Drug resistance
✅ Answer: C
49. Most common route of entry during floods:
A. Inhalation
B. Ingestion
C. Through skin abrasions
D. Vector bite
✅ Answer: C
50. Best strategy to reduce leptospirosis burden:
A. Mass vaccination
B. Early diagnosis and prevention
C. Isolation only
D. Antibiotic prophylaxis for all
✅ Answer: B
