Introduction
-
Cryptococcosis is a serious opportunistic fungal infection caused by encapsulated yeasts of the genus Cryptococcus.
-
The two most important pathogenic species responsible for human infection are Cryptococcus neoformans and Cryptococcus gattii.
-
These fungi are widely distributed in the environment, especially in soil contaminated with pigeon droppings, decaying organic matter, and certain tree species.
-
Humans usually acquire the infection through inhalation of airborne yeast cells or fungal spores present in the environment.
-
Cryptococcosis mainly affects immunocompromised individuals, including patients with HIV/AIDS, organ transplant recipients, cancer patients, and individuals receiving immunosuppressive therapy.
-
Unlike Cryptococcus neoformans, Cryptococcus gattii can also infect immunocompetent individuals.
-
The infection usually begins in the lungs following inhalation of the organism and may remain localized or spread to other organs through the bloodstream.
-
The central nervous system (CNS) is the most common site of dissemination, often leading to cryptococcal meningitis, a severe and potentially life-threatening condition.
-
Diagnosis of cryptococcosis requires a combination of clinical evaluation, microscopic examination, culture methods, antigen detection tests, and molecular diagnostic techniques.
Signs and Symptoms
The signs and symptoms of cryptococcosis depend on the site of infection and the immune status of the patient. The infection most commonly affects the lungs and central nervous system.
General Symptoms
Common symptoms seen in many patients include:
-
Fever
-
Fatigue
-
Weight loss
-
Weakness
-
Night sweats
Pulmonary Cryptococcosis (Lung Infection)
When the infection affects the lungs, the symptoms may include:
-
Persistent cough
-
Chest pain
-
Shortness of breath
-
Fever
-
Production of sputum
In some individuals, pulmonary infection may be asymptomatic and detected incidentally during imaging studies.
Cryptococcal Meningitis (CNS Infection)
When the infection spreads to the central nervous system, it can cause cryptococcal meningitis, which presents with:
-
Severe headache
-
Fever
-
Neck stiffness
-
Nausea and vomiting
-
Sensitivity to light (photophobia)
-
Altered mental status
-
Confusion or memory problems
If untreated, cryptococcal meningitis can lead to coma and death.
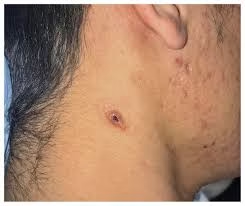
Cutaneous Cryptococcosis
Skin involvement may present as:
-
Skin nodules
-
Ulcerated lesions
-
Cellulitis-like lesions
-
Papules or pustules
Disseminated Cryptococcosis
In severe cases, the infection spreads to multiple organs, leading to symptoms such as:
-
Multi-organ involvement
-
Severe systemic infection
-
Neurological complications
Early recognition of symptoms and prompt laboratory diagnosis are essential for effective treatment and prevention of complications.
Causes
Cryptococcosis is caused by encapsulated yeasts of the genus Cryptococcus. Infection occurs when environmental fungal cells enter the body, usually through inhalation.
Main Causes
-
Cryptococcus neoformans
-
The most common cause of cryptococcosis worldwide.
-
Commonly found in soil contaminated with pigeon droppings, bird excreta, and decaying organic matter.
-
Mainly infects immunocompromised individuals such as patients with HIV/AIDS.
-
-
Cryptococcus gattii
-
Often associated with soil and certain tree species, particularly eucalyptus trees.
-
More common in tropical and subtropical regions.
-
Can infect both immunocompetent and immunocompromised individuals.
-
Mode of Transmission
-
Infection occurs mainly through inhalation of airborne yeast cells or spores from contaminated environmental sources.
-
After entering the lungs, the organism may remain localized or spread through the bloodstream to other organs, especially the brain.
Risk Factors
Certain conditions increase the risk of developing cryptococcosis:
-
HIV/AIDS
-
Organ transplantation
-
Cancer chemotherapy
-
Long-term corticosteroid therapy
-
Immunosuppressive drugs
-
Chronic diseases affecting immunity
Etiology
Cryptococcosis is mainly caused by two species of the genus Cryptococcus. Each species differs in ecological niche, host susceptibility, and geographic distribution.
| Species | Key Characteristics | Common Sources | Typical Hosts |
|---|---|---|---|
| Cryptococcus neoformans | Most common cause of cryptococcosis worldwide | Pigeon droppings, soil, decaying wood | Primarily immunocompromised individuals |
| Cryptococcus gattii | Often infects immunocompetent individuals | Soil and eucalyptus trees | Both immunocompetent and immunocompromised hosts |
Cryptococcus neoformans
-
The most common cause of cryptococcal infection
-
Associated with pigeon droppings and contaminated soil
-
Frequently causes pulmonary infection followed by dissemination to the CNS
Cryptococcus gattii
-
Found mainly in tropical and subtropical regions
-
Associated with trees, especially eucalyptus
-
Can cause infection in healthy individuals
Clinical Specimens
The type of clinical specimen collected depends on the site of infection.
| Specimen | Clinical Indication |
|---|---|
| Cerebrospinal Fluid (CSF) | Suspected cryptococcal meningitis |
| Blood | Disseminated cryptococcosis |
| Sputum / BAL fluid | Pulmonary cryptococcosis |
| Tissue biopsy | Deep systemic infection |
| Urine | Rare urinary tract infection |
| Skin scrapings | Cutaneous cryptococcosis |
Among these, CSF is the most important specimen in cases of cryptococcal meningitis.
Direct Microscopic Examination
Microscopic examination of clinical specimens is often the first step in laboratory diagnosis.
| Method | Principle | Diagnostic Feature |
|---|---|---|
| India Ink Preparation | Negative staining technique | Capsule appears as a clear halo around yeast cells |
| Gram Stain | Standard staining method | Round budding Gram-positive yeast cells |
| Mucicarmine Stain | Capsule-specific stain | Capsule appears bright red |
| KOH Preparation | Dissolves background material | Yeast cells visible with capsule |
| Hematoxylin & Eosin (H&E) | Histopathological examination | Encapsulated yeast in tissue sections |
India Ink Staining
India ink staining is a rapid and classical diagnostic method used mainly for CSF samples. The thick capsule surrounding Cryptococcus cells excludes the ink, producing a distinct clear halo around the yeast cell.
Culture and Identification
Culture remains the gold standard for confirming cryptococcal infection.
Culture Media Used
| Culture Medium | Purpose |
|---|---|
| Sabouraud Dextrose Agar (SDA) | General fungal growth |
| Bird Seed Agar (Niger seed agar) | Selective medium for Cryptococcus |
Colony Characteristics
| Feature | Description |
|---|---|
| Appearance | Smooth, creamy colonies |
| Color | White to cream |
| Texture | Often mucoid due to capsule |
| Growth time | 2–5 days |
Biochemical Identification
Key biochemical tests include:
-
Urease test – positive
-
Carbohydrate assimilation tests
-
Phenol oxidase production
Antigen Detection
Detection of cryptococcal antigen (CrAg) in clinical specimens is one of the most sensitive diagnostic methods.
Common techniques include:
-
Latex agglutination tests
-
Lateral flow assays
-
Enzyme immunoassays
These tests can be performed on:
-
CSF
-
Serum
-
Urine
-
Other body fluids
Molecular Methods
Polymerase Chain Reaction (PCR) is increasingly used for:
-
Rapid detection of fungal DNA
-
Species identification
-
Diagnosis in culture-negative cases
Other Laboratory Investigations
Several additional tests help confirm diagnosis and assess disease severity.
| Test | Purpose |
|---|---|
| Cryptococcal antigen test (CrAg) | Rapid detection of fungal capsule antigen |
| Serological tests | Detection of antibodies |
| Antifungal susceptibility testing | Guides treatment in severe cases |
| Imaging studies | Detect organ involvement |
Imaging Studies
-
Chest X-ray or CT scan → pulmonary cryptococcosis
-
Brain MRI or CT scan → cryptococcal meningitis
Pathogenesis
The pathogenicity of Cryptococcus depends on several virulence factors that help the organism survive in the host and evade immune responses.
Major Virulence Factors
| Virulence Factor | Function |
|---|---|
| Polysaccharide capsule | Prevents phagocytosis and immune recognition |
| Melanin production | Protects against oxidative stress |
| Thermotolerance | Enables growth at human body temperature |
| CNS invasion ability | Allows penetration of blood–brain barrier |
Disease Development
-
Infection begins after inhalation of fungal cells.
-
Initial infection occurs in the lungs.
-
In immunocompromised individuals, the fungus may disseminate through the bloodstream.
-
The organism often reaches the central nervous system, causing cryptococcal meningitis.
Treatment
Treatment depends on the severity of infection and immune status of the patient.
Antifungal Treatment Regimens
| Treatment Phase | Drugs Used | Purpose |
|---|---|---|
| Induction Therapy | Amphotericin B + Flucytosine | Rapid fungal clearance |
| Consolidation Therapy | Fluconazole | Prevent relapse |
| Maintenance Therapy | Long-term Fluconazole | Prevent recurrence |
Amphotericin B
-
Binds to ergosterol in fungal cell membrane
-
Causes cell membrane damage and fungal death
Flucytosine
-
Inhibits fungal DNA synthesis
-
Often used in combination with amphotericin B
Fluconazole
-
Inhibits ergosterol synthesis
-
Used for long-term therapy and prevention of relapse
Prophylaxis
In HIV/AIDS patients, prophylactic fluconazole may be used to prevent cryptococcal infection.
Surgical Management
In some cases, surgical drainage of cryptococcal lesions or abscesses may be required.
MCQs
1. Cryptococcosis is caused by which type of organism?
A. Bacteria
B. Virus
C. Fungus
D. Parasite
Answer: C. Fungus
2. The most common species causing cryptococcosis is:
A. Candida albicans
B. Cryptococcus neoformans
C. Aspergillus fumigatus
D. Histoplasma capsulatum
Answer: B. Cryptococcus neoformans
3. Cryptococcus species are:
A. Filamentous fungi
B. Encapsulated yeast
C. Bacteria
D. Protozoa
Answer: B. Encapsulated yeast
4. The major virulence factor of Cryptococcus is:
A. Capsule
B. Flagella
C. Pili
D. Hyphae
Answer: A. Capsule
5. The natural reservoir of Cryptococcus neoformans is:
A. Freshwater
B. Soil contaminated with pigeon droppings
C. Human skin
D. Plants
Answer: B. Soil contaminated with pigeon droppings
6. Cryptococcus infection occurs mainly through:
A. Ingestion
B. Inhalation
C. Skin contact
D. Blood transfusion
Answer: B. Inhalation
7. The primary site of infection is usually:
A. Skin
B. Lungs
C. Intestine
D. Liver
Answer: B. Lungs
8. The most serious manifestation of cryptococcosis is:
A. Skin infection
B. Pneumonia
C. Meningitis
D. Sinusitis
Answer: C. Meningitis
9. Cryptococcal meningitis is most common in:
A. Healthy adults
B. HIV/AIDS patients
C. Children
D. Pregnant women
Answer: B. HIV/AIDS patients
10. Which staining technique is commonly used to detect Cryptococcus in CSF?
A. Gram stain
B. India ink stain
C. Acid-fast stain
D. Wright stain
Answer: B. India ink stain
11. In India ink preparation, the capsule appears as:
A. Dark stain
B. Clear halo around yeast cell
C. Filamentous structure
D. Pink spores
Answer: B. Clear halo around yeast cell
12. The capsule of Cryptococcus is composed mainly of:
A. Protein
B. Lipid
C. Polysaccharide
D. Peptidoglycan
Answer: C. Polysaccharide
13. The best specimen for diagnosing cryptococcal meningitis is:
A. Urine
B. Blood
C. Cerebrospinal fluid
D. Stool
Answer: C. Cerebrospinal fluid
14. Which culture medium is used to grow Cryptococcus?
A. Nutrient agar
B. Sabouraud dextrose agar
C. MacConkey agar
D. Chocolate agar
Answer: B. Sabouraud dextrose agar
15. Cryptococcus colonies on culture are typically:
A. Dry
B. Cottony
C. Creamy and mucoid
D. Pigmented black
Answer: C. Creamy and mucoid
16. Bird seed agar helps detect:
A. Capsule formation
B. Melanin production
C. Hyphae formation
D. Spores
Answer: B. Melanin production
17. Cryptococcus produces which enzyme?
A. Coagulase
B. Catalase
C. Urease
D. Oxidase
Answer: C. Urease
18. Cryptococcal antigen test detects:
A. Cell wall protein
B. Capsule polysaccharide
C. DNA
D. Lipid
Answer: B. Capsule polysaccharide
19. The most sensitive diagnostic test for cryptococcosis is:
A. Microscopy
B. Culture
C. Antigen detection
D. Gram stain
Answer: C. Antigen detection
20. Cryptococcus gattii is commonly associated with:
A. Pine trees
B. Eucalyptus trees
C. Coconut trees
D. Mango trees
Answer: B. Eucalyptus trees
21. Cryptococcus gattii infection can occur in:
A. Only immunocompromised patients
B. Only elderly patients
C. Immunocompetent individuals
D. Only children
Answer: C. Immunocompetent individuals
22. The antifungal drug used in induction therapy is:
A. Amphotericin B
B. Penicillin
C. Tetracycline
D. Ciprofloxacin
Answer: A. Amphotericin B
23. Amphotericin B is commonly combined with:
A. Fluconazole
B. Flucytosine
C. Ketoconazole
D. Itraconazole
Answer: B. Flucytosine
24. Maintenance therapy commonly uses:
A. Amphotericin B
B. Fluconazole
C. Nystatin
D. Terbinafine
Answer: B. Fluconazole
25. Cryptococcus grows well at:
A. 10°C
B. 20°C
C. 37°C
D. 50°C
Answer: C. 37°C
26. Melanin production in Cryptococcus helps in:
A. Capsule formation
B. Immune evasion
C. Sporulation
D. Growth
Answer: B. Immune evasion
27. Cryptococcus cells reproduce by:
A. Binary fission
B. Budding
C. Fragmentation
D. Sporulation
Answer: B. Budding
28. Which staining method highlights capsule in tissue sections?
A. Gram stain
B. Mucicarmine stain
C. Acid-fast stain
D. Wright stain
Answer: B. Mucicarmine stain
29. The infection spreads to CNS mainly through:
A. Lymph nodes
B. Bloodstream
C. Skin
D. Intestine
Answer: B. Bloodstream
30. Pulmonary cryptococcosis commonly presents with:
A. Rash
B. Persistent cough
C. Diarrhea
D. Joint pain
Answer: B. Persistent cough
31. Neck stiffness is a symptom of:
A. Pneumonia
B. Meningitis
C. Skin infection
D. Kidney disease
Answer: B. Meningitis
32. Headache in cryptococcosis indicates involvement of:
A. Lungs
B. Skin
C. CNS
D. Liver
Answer: C. CNS
33. PCR is used for:
A. Culture growth
B. DNA detection
C. Capsule staining
D. Antigen detection
Answer: B. DNA detection
34. Cryptococcus belongs to which fungal group?
A. Basidiomycetes
B. Ascomycetes
C. Zygomycetes
D. Deuteromycetes
Answer: A. Basidiomycetes
35. Which body fluid is commonly used for antigen detection?
A. CSF
B. Saliva
C. Sweat
D. Tears
Answer: A. CSF
36. Cutaneous cryptococcosis may appear as:
A. Nodules
B. Ulcers
C. Papules
D. All of the above
Answer: D. All of the above
37. The incubation period of cryptococcosis is:
A. Minutes
B. Hours
C. Days to weeks
D. Years
Answer: C. Days to weeks
38. Cryptococcus is classified as:
A. Bacteria
B. Yeast-like fungus
C. Virus
D. Protozoa
Answer: B. Yeast-like fungus
39. Which test is rapid for diagnosis?
A. India ink test
B. Culture
C. PCR
D. Biopsy
Answer: A. India ink test
40. Capsule helps Cryptococcus to:
A. Move faster
B. Resist immune response
C. Produce toxins
D. Form spores
Answer: B. Resist immune response
41. Disseminated cryptococcosis means infection of:
A. Only lungs
B. Multiple organs
C. Only skin
D. Only brain
Answer: B. Multiple organs
42. Fever in cryptococcosis occurs due to:
A. Immune response
B. Capsule formation
C. Melanin production
D. Growth temperature
Answer: A. Immune response
43. Which imaging method is used in pulmonary infection?
A. Chest X-ray
B. MRI brain
C. Ultrasound
D. ECG
Answer: A. Chest X-ray
44. MRI is useful for detecting:
A. Lung infection
B. Brain involvement
C. Skin lesions
D. Liver infection
Answer: B. Brain involvement
45. Which patient group is most susceptible?
A. Athletes
B. HIV patients
C. Healthy adults
D. Children
Answer: B. HIV patients
46. Cryptococcus cells appear as:
A. Rod-shaped bacteria
B. Round budding yeast
C. Spiral bacteria
D. Filamentous molds
Answer: B. Round budding yeast
47. The disease spreads mainly by:
A. Airborne route
B. Food
C. Water
D. Skin contact
Answer: A. Airborne route
48. Early diagnosis helps prevent:
A. Fever
B. CNS complications
C. Skin rash
D. Diarrhea
Answer: B. CNS complications
49. Antifungal susceptibility testing helps in:
A. Diagnosing infection
B. Selecting effective treatment
C. Detecting capsule
D. Identifying spores
Answer: B. Selecting effective treatment
50. Cryptococcosis is classified as:
A. Opportunistic fungal infection
B. Viral infection
C. Bacterial infection
D. Parasitic infection
Answer: A. Opportunistic fungal infection
