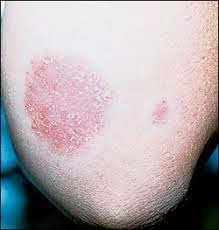
Superficial dermatophyte infections involve the skin, hair, or nails and are caused by dermatophytes belonging to genera such as Trichophyton, Microsporum, and Epidermophyton. Laboratory diagnosis relies on microscopy, culture, and adjunctive techniques to confirm and identify the fungal pathogen. Below is a detailed breakdown of the diagnostic approach.
Microscopic Examination
Microscopy is a rapid diagnostic tool used to detect fungal elements directly from clinical samples.
Sample Collection
The quality of the specimen is critical for accurate diagnosis.
- Skin scrapings: Taken from the active edge of the lesion using a sterile blade or scalpel.
- Hair samples: Plucked from the affected area, preferably including the root and shafts. Broken or lusterless hairs are targeted.
- Nail clippings: Collected from discolored or brittle portions of the nail, including the subungual debris.
Sample Preparation
- KOH Preparation:
- A 10–20% potassium hydroxide (KOH) solution is added to the sample on a glass slide.
- The slide is gently heated to dissolve keratin, exposing fungal structures.
- The preparation is examined under a light microscope.
- Enhancements for visualization:
- Chlorazol Black E stain: Highlights fungal hyphae with contrasting colors.
- Calcofluor White stain: A fluorescent dye binds to fungal cell walls, allowing visualization under UV light or a fluorescence microscope.
Procedure
- Specimen Collection:
- Use a sterile blade or scalpel to scrape the skin from the advancing edge of lesions.
- For hair, pluck brittle, lustrous, or broken hairs.
- For nails, collect discolored, thickened, or brittle parts and subungual debris.
- Place the specimen in a sterile container to avoid contamination.
- Preparation:
- Mount the sample on a clean glass slide.
- Add 1–2 drops of 10–20% Potassium Hydroxide (KOH) to digest keratin and expose fungal elements.
- Cover the sample with a coverslip.
- Gently heat over a flame or slide warmer (not boiling).
- Optional: Let it stand at room temperature for 10–30 minutes without heating.
- Enhance visualization by adding Chlorazol Black E or Calcofluor White stain:
- Chlorazol Black E: Binds to fungal cell walls, highlighting hyphae in dark green/black.
- Calcofluor White: Binds chitin, fluorescing fungal elements under UV light.
- Examination:
- Use a light microscope under low power (10x) and high power (40x).
- For Calcofluor White, use a fluorescence microscope.
Results Interpretation
- Positive Results:
- Skin: Thin, branching, septate hyphae with uniform width.
- Hair:
- Ectothrix: Hyphae and arthroconidia outside the hair shaft.
- Endothrix: Hyphae and arthroconidia within the hair shaft.
- Nails: Irregularly shaped, fragmented hyphae and occasional spores.
- Negative Results:
- Absence of fungal structures. May require culture for confirmation.
Advantages and Limitations
- Advantages:
- Rapid (results within minutes to hours).
- Cost-effective.
- Limitations:
- Low sensitivity if fungal elements are sparse.
- Requires experienced interpretation.
Culture
Culture is the gold standard for identifying dermatophyte species and evaluating antifungal susceptibility.
Specimen Inoculation
- Specimens are inoculated onto fungal growth media such as:
- Sabouraud Dextrose Agar (SDA): Enriched with antibiotics (e.g., chloramphenicol, gentamicin) to suppress bacterial contaminants. Cycloheximide is added to inhibit non-dermatophyte fungi.
- Dermatophyte Test Medium (DTM): Contains phenol red as a pH indicator that turns red when dermatophytes metabolize keratin.
- Mycosel Agar: Selective for dermatophytes due to the presence of cycloheximide and antibiotics.
Incubation
- Plates are incubated at 25–30°C for 2–4 weeks.
- Dermatophytes are slow-growing; some species require prolonged incubation to develop distinct colonies.
Identification of Dermatophytes
- Colony Morphology:
- Surface texture: Powdery, velvety, or cottony.
- Pigmentation: The surface and reverse side of the colony show species-specific colors (e.g., white, yellow, or brown).
Procedure
- Specimen Preparation:
- Ensure adequate and sterile collection of skin, hair, or nail samples.
- Media for Culture:
- Sabouraud Dextrose Agar (SDA):
- Add antibiotics (chloramphenicol or gentamicin) to inhibit bacterial growth.
- Add cycloheximide to inhibit saprophytic fungi.
- Dermatophyte Test Medium (DTM):
- Contains a phenol red indicator that changes color to red if dermatophytes metabolize keratin.
- Mycosel Agar:
- Used to selectively isolate dermatophytes.
- Sabouraud Dextrose Agar (SDA):
- Inoculation:
- Divide the specimen into small fragments and press them lightly onto the culture media.
- Avoid embedding the sample too deeply into the agar.
- Incubation:
- Place plates in an incubator at 25–30°C.
- Monitor for growth every 3–7 days, continuing for up to 4 weeks to ensure detection of slow-growing fungi.
- Colony Observation:
- Surface Morphology: Powdery, velvety, or cottony texture; species-dependent color.
- Reverse Pigmentation: Pigment on the underside of the colony varies by species.
- Transfer a colony fragment for Lactophenol Cotton Blue (LPCB) staining:
- Examine macroconidia and microconidia microscopically for species identification.
Results Interpretation
- Positive Results:
- Trichophyton rubrum: Fluffy white colonies with deep red reverse pigmentation. Tear-drop microconidia.
- Microsporum canis: Cottony white colonies with yellow reverse. Spindle-shaped macroconidia.
- Epidermophyton floccosum: Suede-like yellow-brown colonies with club-shaped macroconidia.
- Negative Results:
- No fungal growth after 4 weeks.
Advantages and Limitations
- Advantages:
- Species-level identification.
- Allows antifungal susceptibility testing.
- Limitations:
- Time-consuming (2–4 weeks).
- Requires proper storage and transportation of samples.
- Microscopic Examination of Culture:
- A small portion of the colony is stained using Lactophenol Cotton Blue.
- Characteristic features include:
- Macroconidia: Large, spindle- or cigar-shaped, with septations (e.g., Microsporum species).
- Microconidia: Small, round to tear-drop shaped, often found in clusters (e.g., Trichophyton species).
Common Dermatophytes Identified
- Trichophyton rubrum: White fluffy colonies, red reverse pigmentation, teardrop-shaped microconidia.
- Microsporum canis: Cottony white surface, yellow reverse pigmentation, spindle-shaped macroconidia.
- Epidermophyton floccosum: Yellow-brown colonies with club-shaped macroconidia and no microconidia.
Additional Diagnostic Techniques
Wood’s Lamp Examination
- A UV light source emitting at 365 nm is used to examine affected areas.
- Hair infected with some Microsporum species fluoresces greenish-yellow (e.g., M. canis).
Histopathology
- Skin or nail biopsies stained with Periodic Acid-Schiff (PAS) or Gomori Methenamine Silver can detect tissue fungal elements.
- Useful for deeper infections where scraping yields inadequate samples.
Molecular Techniques
- Polymerase Chain Reaction (PCR): Detects fungal DNA directly from samples and is highly sensitive.
- DNA sequencing and MALDI-TOF mass spectrometry help identify species in atypical cases.
Antifungal Susceptibility Testing
- Performed for recurrent or treatment-resistant cases using specialized fungal culture techniques or molecular methods.
Advantages and Limitations
Microscopy
- Advantages: Quick, inexpensive, non-culture dependent.
- Limitations: Low sensitivity; requires experienced interpretation.
Culture
- Advantages: Gold standard; allows species identification and antifungal testing.
- Limitations: Time-consuming (weeks for results), contamination risk.
Advanced Methods
- Advantages: High sensitivity and specificity (e.g., PCR).
- Limitations: Expensive and less available in routine clinical settings.