Introduction
-
Gram-negative, aerobic, non-fermenting bacillus
-
Widely distributed in nature; found in soil, water, and moist environments
-
Important opportunistic pathogen in humans
-
Common cause of hospital-acquired (nosocomial) infections
-
Causes severe infections in immunocompromised patients, burn patients, neonates, and those with chronic diseases
-
Has minimal nutritional requirements and survives in adverse conditions
-
Produces characteristic pigments such as pyocyanin and pyoverdin
-
Emits a fruity or grape-like odor
-
Capable of growth at 42°C
-
Forms biofilms, especially on medical devices
-
Shows intrinsic and acquired multidrug resistance
-
Causes infections such as pneumonia, wound and burn infections, urinary tract infections, septicemia, otitis externa, and keratitis
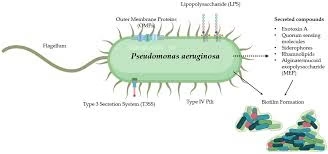
General Character
Genus: Pseudomonas
Species: Pseudomonas aeruginosa
Family: Pseudomonadaceae
Gram staining:
- Gram-negative bacillus
- Appears as slender, straight rods
- Stains pink due to a thin peptidoglycan layer and the presence of an outer membrane
Shape and arrangement:
- Rod-shaped (bacilli)
- Usually seen singly or in pairs
- Non-spore forming
Motility:
- Actively motile
- Possesses a single polar flagellum (monotrichous)
Oxygen requirement:
- Obligate aerobe (strict aerobe)
- Can survive under low oxygen tension by using nitrate as an alternative electron acceptor
Capsule:
- Capsule may be present, especially in chronic infections
- Mucoid strains produce alginate, particularly seen in cystic fibrosis patients
- Alginate contributes to biofilm formation and virulence
Morphology
Pseudomonas aeruginosa is a Gram-negative, non-spore-forming bacillus with characteristic morphological features that are helpful for laboratory identification.
Shape and size
-
Slender, straight to slightly curved rod-shaped bacterium
-
Measures approximately 1.5–3.0 µm in length and 0.5–0.8 µm in width
-
Commonly seen as single cells, occasionally in pairs
Gram staining
-
Gram-negative, appearing pink to red on Gram staining
-
Possesses a thin peptidoglycan layer and an outer membrane containing lipopolysaccharide (LPS)
Motility
-
Motile organism
-
Possesses a single polar (monotrichous) flagellum
-
Motility can be demonstrated by hanging drop preparation
Capsule and slime layer
-
Usually non-capsulated
-
Produces an extracellular slime layer (alginate) in many strains
-
Mucoid strains are commonly associated with chronic infections, especially in cystic fibrosis
Spores
-
Non-spore-forming
Arrangement
-
Cells are usually arranged singly, rarely in pairs
-
No characteristic chain or cluster formation
Special morphological features
-
Presence of pili (fimbriae) aiding in adhesion
-
Ability to form biofilms, an important morphological and pathogenic feature
Cultural Characteristics
Pseudomonas aeruginosa shows distinctive growth patterns on routine and selective media, which are very useful for laboratory identification.
Growth requirements
-
Strictly aerobic organism
-
Grows well at 37°C (optimum)
-
Can grow at 42°C, which helps differentiate it from many other non-fermenters
-
Simple nutritional requirements
Nutrient agar
-
Produces large, flat, irregular colonies
-
Colonies have a metallic sheen
-
Characteristic grape-like or corn taco odor (due to aminoacetophenone)
-
Pigment production may cause blue-green discoloration of the medium
Blood agar
-
Forms large, spreading colonies
-
Often shows β-hemolysis
-
Pigment may diffuse into the surrounding medium
MacConkey agar
-
Produces non-lactose fermenting colonies
-
Colonies appear pale or colorless
-
Medium may show slight greenish pigmentation due to pyocyanin
Cetrimide agar (selective medium)
-
Selective for Pseudomonas aeruginosa
-
Shows enhanced blue-green pigmentation (pyocyanin and fluorescein)
-
Colonies are well-defined and easy to identify
Pigment production
-
Produces several characteristic pigments:
-
Pyocyanin – blue-green (specific for P. aeruginosa)
-
Pyoverdin (fluorescein) – yellow-green, fluorescent under UV light
-
Pyorubin – red
-
Pyomelanin – brown to black
-
Odor
-
Produces a characteristic fruity or grape-like smell
Mucoid colonies
-
In chronic infections (e.g., cystic fibrosis), colonies appear large, glistening, and mucoid due to alginate production
Biochemical Reactions
The biochemical reaction pattern of Pseudomonas aeruginosa is characteristic and helps in its definitive laboratory identification.
Oxidase test
-
Positive
-
Rapid development of dark purple color
-
Important test to differentiate from Enterobacteriaceae
Catalase test
-
Positive
-
Shows immediate effervescence on addition of hydrogen peroxide
Carbohydrate utilization
-
Non-fermenter of carbohydrates
-
Glucose is utilized oxidatively, not fermentatively
-
Demonstrated by oxidative–fermentative (O/F) test:
-
Open tube: acid production (yellow)
-
Closed tube: no change (green)
-
Indole test
-
Negative
Methyl red test
-
Negative
Voges–Proskauer test
-
Negative
Citrate utilization test
-
Positive (uses citrate as sole carbon source)
Urease test
-
Negative (usually)
Nitrate reduction test
-
Positive
-
Reduces nitrate to nitrite and often to nitrogen gas
Triple sugar iron (TSI) agar
-
No fermentation of sugars
-
Alkaline slant / no change in butt (K/NC)
-
No gas, no H₂S
Gelatin liquefaction
-
Positive (rapid gelatin hydrolysis)
Arginine dihydrolase test
-
Positive
Acetamide utilization test
-
Positive (highly characteristic for P. aeruginosa)
Pathogenicity
Pseudomonas aeruginosa is an opportunistic pathogen capable of causing a wide range of infections, particularly in immunocompromised patients, hospitalized individuals, and those with breaches in normal host defenses.
General pathogenic features
-
Low intrinsic virulence but causes severe disease when host immunity is compromised
-
Commonly associated with nosocomial infections
-
Exhibits multidrug resistance, contributing to persistent and difficult-to-treat infections
Virulence factors
Adhesins
-
Pili (fimbriae) facilitate attachment to epithelial cells
-
Alginate slime layer aids in adherence and biofilm formation
Toxins
-
Exotoxin A
-
Inhibits protein synthesis by ADP-ribosylation of elongation factor-2 (EF-2)
-
Mechanism similar to diphtheria toxin
-
Causes tissue necrosis and immunosuppression
-
-
Exoenzymes (Type III secretion system)
-
Exoenzyme S – interferes with host cell signaling and cytoskeleton
-
Exoenzyme T – disrupts actin polymerization
-
Exoenzyme U – cytotoxic, causes rapid cell death
-
Exoenzyme Y – increases intracellular cAMP
-
Enzymes
-
Elastase – destroys elastin, collagen, immunoglobulins, and complement
-
Alkaline protease – degrades host tissues and immune components
-
Phospholipase C – damages cell membranes and surfactant
Pigments
-
Pyocyanin
-
Generates reactive oxygen species
-
Impairs ciliary function and neutrophil activity
-
-
Pyoverdin
-
Acts as a siderophore for iron acquisition
-
Endotoxin
-
Lipopolysaccharide (LPS)
-
Causes fever, inflammation, septic shock
-
Biofilm formation
-
Produces alginate, forming biofilms on tissues and medical devices
-
Biofilms protect bacteria from antibiotics and host immune responses
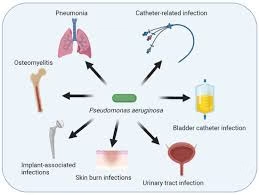
Clinical manifestations
Respiratory infections
-
Ventilator-associated pneumonia
-
Chronic lung infection in cystic fibrosis patients
Skin and soft tissue infections
-
Wound and burn infections (blue-green pus)
-
Hot tub folliculitis
Ear and eye infections
-
Otitis externa, including malignant otitis externa
-
Keratitis and corneal ulcers, especially in contact lens users
Urinary tract infections
-
Catheter-associated UTIs
Bloodstream infections
-
Septicemia, especially in neutropenic patients
-
Characteristic skin lesion: ecthyma gangrenosum
Other infections
-
Osteomyelitis (post puncture wounds)
-
Endocarditis in IV drug users
Laboratory Diagnosis
Specimen collection
-
Pus or wound swab (burns, surgical site infections)
-
Sputum or endotracheal aspirate (pneumonia, ventilator-associated infections)
-
Urine (catheter-associated urinary tract infections)
-
Blood (septicemia)
-
Ear discharge (otitis externa)
-
Corneal scrapings (keratitis)
Direct microscopy
-
Gram staining of clinical specimen shows Gram-negative bacilli
-
Numerous pus cells may be seen
-
Motility can be demonstrated by hanging drop preparation
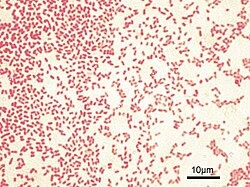
Culture methods
Primary culture media
-
Nutrient agar: large, flat colonies with metallic sheen and blue-green pigmentation
-
Blood agar: large colonies, often β-hemolytic
-
MacConkey agar: non-lactose fermenting, pale colonies
Selective medium
-
Cetrimide agar
-
Selective for P. aeruginosa
-
Enhances production of pyocyanin and fluorescein
-
Pigment detection
-
Blue-green pigment (pyocyanin) diffusing into the medium
-
Yellow-green fluorescence (pyoverdin) under UV light
Characteristic odor
-
Fruity or grape-like smell (aminoacetophenone)
Biochemical identification
-
Oxidase test: positive
-
Catalase test: positive
-
O/F glucose test: oxidative
-
Citrate utilization: positive
-
Nitrate reduction: positive
-
Acetamide utilization: positive
-
Indole, MR, VP: negative
Temperature test
-
Growth at 42°C, helping to differentiate from other non-fermenters
Antibiotic susceptibility testing
-
Essential due to intrinsic and acquired drug resistance
-
Performed by Kirby–Bauer disc diffusion, MIC determination, or automated systems
-
Detection of multidrug-resistant (MDR) strains is clinically important
Molecular methods (advanced laboratories)
-
PCR for rapid identification and resistance genes
-
Useful in outbreak investigations
Antibiotic Resistance
Pseudomonas aeruginosa is notorious for its intrinsic, acquired, and adaptive resistance mechanisms, making it one of the most challenging pathogens to treat in clinical practice.
Intrinsic resistance
-
Low outer membrane permeability, limiting antibiotic entry
-
Presence of multidrug efflux pumps (e.g., MexAB-OprM, MexXY)
-
Naturally resistant to many antibiotics, including:
-
Penicillin G
-
First- and second-generation cephalosporins
-
Macrolides
-
Tetracyclines
-
Chloramphenicol
-
Enzymatic resistance
β-lactamases
-
Produces AmpC β-lactamase, conferring resistance to many β-lactam antibiotics
-
Can acquire extended-spectrum β-lactamases (ESBLs)
-
May produce carbapenemases (e.g., metallo-β-lactamases such as VIM, IMP, NDM)
Aminoglycoside-modifying enzymes
-
Acetylation, phosphorylation, or adenylation of aminoglycosides, reducing drug activity
Target site modifications
-
Alteration of DNA gyrase or topoisomerase IV, leading to fluoroquinolone resistance
-
Modification or loss of OprD porin, causing resistance to imipenem
Efflux pump overexpression
-
Upregulation of efflux systems expels multiple classes of antibiotics, including:
-
β-lactams
-
Fluoroquinolones
-
Aminoglycosides
-
Biofilm-associated resistance
-
Biofilm formation markedly reduces antibiotic penetration
-
Bacteria within biofilms exhibit slow growth and altered metabolism, reducing antibiotic efficacy
-
Common in chronic lung infections and device-related infections
Adaptive resistance
-
Temporary resistance during antibiotic exposure
-
Reversible once selective pressure is removed
Multidrug-resistant (MDR) and extensively drug-resistant (XDR) strains
-
MDR strains: resistant to at least one agent in three or more antimicrobial classes
-
XDR strains: susceptible to only one or two classes
-
Major concern in ICU and hospital settings
Clinical significance
-
Limits therapeutic options
-
Requires antibiotic susceptibility testing before treatment
-
Often necessitates combination therapy
Prevention
Prevention of Pseudomonas aeruginosa infection primarily focuses on infection control measures, hospital hygiene, and protection of high-risk patients, as no effective vaccine is currently available.
General preventive measures
-
Strict adherence to hand hygiene by healthcare workers
-
Proper sterilization and disinfection of medical and surgical instruments
-
Use of aseptic techniques during invasive procedures
Hospital infection control
-
Regular cleaning and disinfection of hospital environment, especially moist areas such as sinks, ventilators, and humidifiers
-
Proper maintenance of ventilators, nebulizers, catheters, and dialysis equipment
-
Surveillance for nosocomial infections, particularly in ICUs
Patient-related measures
-
Careful management of burn wounds and surgical sites
-
Minimizing the duration of indwelling devices (urinary catheters, IV lines)
-
Prompt removal of unnecessary catheters and drains
Antibiotic stewardship
-
Rational and judicious use of antibiotics to prevent selection of resistant strains
-
Avoidance of unnecessary broad-spectrum antibiotic therapy
-
Regular review of antibiotic policies in hospitals
Isolation precautions
-
Contact precautions for patients infected or colonized with multidrug-resistant strains
-
Cohorting of infected patients when necessary
Environmental control
-
Use of sterile water for respiratory therapy equipment
-
Avoidance of contaminated solutions, disinfectants, and medications
Community prevention
-
Proper care of contact lenses to prevent keratitis
-
Avoidance of poorly maintained swimming pools and hot tubs
Vaccine status
-
No licensed vaccine is currently available against Pseudomonas aeruginosa
MCQs
1. Pseudomonas aeruginosa is a
A. Gram-positive coccus
B. Gram-negative bacillus
C. Gram-positive bacillus
D. Gram-negative coccus
Answer: B
2. Oxygen requirement of P. aeruginosa is
A. Obligate anaerobe
B. Facultative anaerobe
C. Aerobic
D. Microaerophilic
Answer: C
3. P. aeruginosa is best described as
A. Lactose fermenter
B. Non-lactose fermenter
C. Slow lactose fermenter
D. Late lactose fermenter
Answer: B
4. Motility in P. aeruginosa is due to
A. Peritrichous flagella
B. Lophotrichous flagella
C. Monotrichous polar flagellum
D. Non-motile
Answer: C
5. Characteristic odor of P. aeruginosa is
A. Fishy
B. Ammoniacal
C. Fruity or grape-like
D. Putrid
Answer: C
6. Which pigment is specific for P. aeruginosa?
A. Pyoverdin
B. Pyomelanin
C. Pyocyanin
D. Prodigiosin
Answer: C
7. Blue-green pigment of P. aeruginosa is
A. Pyoverdin
B. Pyorubin
C. Pyocyanin
D. Pyomelanin
Answer: C
8. Yellow-green fluorescent pigment is
A. Pyocyanin
B. Pyoverdin
C. Pyomelanin
D. Pyorubin
Answer: B
9. Selective medium for P. aeruginosa is
A. Blood agar
B. MacConkey agar
C. Cetrimide agar
D. TCBS agar
Answer: C
10. Growth at 42°C is characteristic of
A. E. coli
B. Klebsiella pneumoniae
C. Pseudomonas aeruginosa
D. Proteus mirabilis
Answer: C
11. Oxidase reaction of P. aeruginosa is
A. Negative
B. Weakly positive
C. Positive
D. Variable
Answer: C
12. Catalase test of P. aeruginosa is
A. Negative
B. Positive
C. Variable
D. Weak
Answer: B
13. Glucose metabolism in P. aeruginosa is
A. Fermentative
B. Oxidative
C. Non-utilizing
D. Mixed acid
Answer: B
14. O/F test result for glucose shows
A. Both tubes yellow
B. Only closed tube yellow
C. Only open tube yellow
D. Both tubes green
Answer: C
15. Indole test is
A. Positive
B. Negative
C. Variable
D. Weakly positive
Answer: B
16. Citrate utilization test is
A. Negative
B. Variable
C. Positive
D. Weak
Answer: C
17. Nitrate reduction test is
A. Negative
B. Positive
C. Variable
D. Weak
Answer: B
18. Acetamide utilization test is
A. Negative
B. Positive
C. Variable
D. Not done
Answer: B
19. TSI reaction of P. aeruginosa is
A. A/A with gas
B. K/A
C. K/NC
D. A/NC
Answer: C
20. Gelatin liquefaction is
A. Negative
B. Slow positive
C. Rapid positive
D. Variable
Answer: C
21. P. aeruginosa is primarily an
A. Obligate pathogen
B. Commensal
C. Opportunistic pathogen
D. Zoonotic pathogen
Answer: C
22. Most common infection in burn patients is caused by
A. Staphylococcus aureus
B. E. coli
C. Pseudomonas aeruginosa
D. Proteus
Answer: C
23. Major exotoxin of P. aeruginosa is
A. Enterotoxin
B. Exotoxin A
C. Endotoxin
D. Hemolysin
Answer: B
24. Exotoxin A acts by
A. Inhibiting cell wall synthesis
B. Inhibiting protein synthesis
C. Inhibiting DNA synthesis
D. Disrupting cell membrane
Answer: B
25. Mechanism of exotoxin A is similar to
A. Tetanus toxin
B. Botulinum toxin
C. Diphtheria toxin
D. Cholera toxin
Answer: C
26. Type III secretion system delivers
A. Endotoxin
B. Exoenzymes
C. Capsule
D. Flagella
Answer: B
27. Virulence factor responsible for biofilm formation is
A. Pili
B. Alginate
C. LPS
D. Flagella
Answer: B
28. Blue-green pus in wounds is due to
A. Pyoverdin
B. Pyocyanin
C. Pyorubin
D. Melanin
Answer: B
29. Ecthyma gangrenosum is associated with
A. Typhoid
B. Cholera
C. Pseudomonas septicemia
D. Diphtheria
Answer: C
30. Common ear infection caused by P. aeruginosa is
A. Otitis media
B. Otitis interna
C. Otitis externa
D. Mastoiditis
Answer: C
31. Most common hospital reservoir of P. aeruginosa is
A. Dry surfaces
B. Dust
C. Moist environments
D. Air
Answer: C
32. Important resistance mechanism is
A. Capsule
B. Efflux pumps
C. Spore formation
D. Plasmid curing
Answer: B
33. Natural resistance is due to
A. Thick peptidoglycan
B. Low membrane permeability
C. Absence of enzymes
D. Capsule
Answer: B
34. AmpC β-lactamase confers resistance to
A. Macrolides
B. Aminoglycosides
C. β-lactams
D. Glycopeptides
Answer: C
35. Imipenem resistance is due to loss of
A. Capsule
B. Flagella
C. OprD porin
D. LPS
Answer: C
36. Biofilm-associated infections are difficult to treat due to
A. Rapid growth
B. Increased metabolism
C. Reduced antibiotic penetration
D. High toxin production
Answer: C
37. Most important step before treatment is
A. Empirical therapy
B. Gram stain
C. Antibiotic susceptibility testing
D. Serology
Answer: C
38. MDR P. aeruginosa is common in
A. OPD
B. Community
C. ICU
D. Schools
Answer: C
39. Prevention mainly involves
A. Vaccination
B. Hand hygiene
C. Chemoprophylaxis
D. Isolation only
Answer: B
40. Vaccine against P. aeruginosa is
A. Available
B. Under national program
C. Not available
D. Given to ICU patients
Answer: C
41. Specimen for ventilator-associated pneumonia is
A. Throat swab
B. Sputum
C. Endotracheal aspirate
D. Blood only
Answer: C
42. Gram stain shows
A. Gram-positive cocci
B. Gram-negative bacilli
C. Acid-fast bacilli
D. Gram-positive bacilli
Answer: B
43. Colony on MacConkey agar appears
A. Pink
B. Red
C. Colorless
D. Mucoid pink
Answer: C
44. Hemolysis on blood agar is usually
A. Alpha
B. Beta
C. Gamma
D. None
Answer: B
45. Slime layer is important in
A. Motility
B. Sporulation
C. Chronic infection
D. Gram staining
Answer: C
46. Contact lens–related keratitis is commonly caused by
A. Staphylococcus epidermidis
B. Candida albicans
C. Pseudomonas aeruginosa
D. Chlamydia
Answer: C
47. Pigment aiding iron uptake is
A. Pyocyanin
B. Pyoverdin
C. Pyorubin
D. Pyomelanin
Answer: B
48. Endotoxin of P. aeruginosa is
A. Capsule
B. Exotoxin A
C. LPS
D. Alginate
Answer: C
49. Important preventive hospital measure is
A. Daily antibiotics
B. Device sterilization
C. Vitamin supplementation
D. Immunization
Answer: B
50. Pseudomonas aeruginosa belongs to family
A. Vibrionaceae
B. Enterobacteriaceae
C. Pseudomonadaceae
D. Neisseriaceae
Answer: C