Introduction
-
Yersinia is a genus of Gram-negative bacteria belonging to the family Enterobacteriaceae.
-
Members of this genus are short, rod-shaped (coccobacillary) organisms.
-
Yersinia species are facultative anaerobes.
-
The genus includes important human pathogens responsible for enteric and systemic infections.
-
Yersinia pestis is the causative agent of plague, a historically important and potentially fatal disease.
-
Yersinia enterocolitica causes yersiniosis, primarily a gastrointestinal infection.
-
Yersinia species are zoonotic pathogens, with animals acting as natural reservoirs.
-
They can survive and multiply at low temperatures, especially Y. enterocolitica.
-
Pathogenicity is mediated by virulence factors such as capsules, endotoxins, and Yersinia outer proteins (Yops).
-
Yersinia infections remain of significant medical and public health importance worldwide.
General Character
- Genus: Yersinia
- Key Species:
-
Yersinia pestis – causes plague
-
Yersinia enterocolitica – causes yersiniosis
-
- Family:
Enterobacteriaceae - Gram Staining:
Yersinia species are Gram-negative bacteria, appearing pink on Gram staining due to the presence of a thin peptidoglycan layer and an outer membrane. - Shape and Arrangement:
-
Shape: Rod-shaped (bacilli)
-
Arrangement: Typically found as single cells or in short chains
- Oxygen Requirements:
Yersinia species are facultative anaerobes, capable of growing in both the presence and absence of oxygen.
Morphology
-
Size:
Small to medium-sized bacteria, approximately 0.5–0.8 µm × 1–3 µm. -
Shape:
Short, plump rod-shaped (coccobacillary) bacilli. -
Gram Reaction:
Gram-negative, staining pink due to thin peptidoglycan layer and outer membrane. -
Arrangement:
Occur singly, in pairs, or occasionally in short chains. -
Bipolar Staining:
Show characteristic bipolar (safety-pin) appearance, especially in clinical specimens and when stained with Wayson, Giemsa, or Leishman stains. -
Motility:
-
Yersinia pestis: Non-motile
-
Yersinia enterocolitica: Motile at 22–25°C, non-motile at 37°C
-
-
Spores:
Non-spore forming. -
Capsule:
-
Yersinia pestis produces a protein capsule (F1 antigen) at 37°C, contributing to virulence.
-
Other species are generally non-capsulated.
-
-
Flagella:
Present in motile species (Y. enterocolitica) at lower temperatures; absent in Y. pestis.
Cultural Characteristics
-
Oxygen Requirement:
Yersinia species are facultative anaerobes and can grow in the presence or absence of oxygen. -
Temperature Requirement:
Grow over a wide temperature range (4°C–40°C).
Optimal growth occurs at 25–28°C.
Yersinia enterocolitica can multiply at refrigerator temperature (cold enrichment). -
Growth on Ordinary Media:
Grow well on simple media such as nutrient agar and peptone water. -
Blood Agar:
-
Colonies are small, smooth, grayish-white.
-
Yersinia pestis is non-hemolytic.
-
-
MacConkey Agar:
-
Non-lactose fermenting colonies (pale colonies).
-
Y. enterocolitica may show delayed lactose fermentation in some strains.
-
-
Selective Media:
-
CIN agar (Cefsulodin–Irgasan–Novobiocin agar):
Produces characteristic “bull’s-eye” colonies (deep red center with transparent border), especially by Y. enterocolitica.
-
-
Broth Culture:
-
In broth, Y. pestis shows turbidity with flocculent deposits and may form “stalactite growth” when grown undisturbed.
-
-
Special Features:
-
Yersinia pestis grows slowly at 37°C compared to other Enterobacteriaceae.
-
Colony morphology varies with temperature and species.
-
Biochemical Reactions
-
Carbohydrate Fermentation:
-
Glucose: Fermented with acid production only (no gas).
-
Lactose: Not fermented (non-lactose fermenter); some strains of Y. enterocolitica may show delayed fermentation.
-
Sucrose: Usually not fermented (species dependent).
-
Mannitol: Fermented by Y. enterocolitica.
-
-
Oxidase Test: Oxidase negative.
-
Catalase Test: Catalase positive.
-
Indole Test:
-
Yersinia pestis: Indole negative
-
Yersinia enterocolitica: Indole positive (most strains)
-
-
Urease Test:
-
Y. pestis: Urease negative
-
Y. enterocolitica: Urease positive (rapid urease producer)
-
-
Methyl Red (MR) Test: Positive.
-
Voges–Proskauer (VP) Test: Negative.
-
Citrate Utilization: Negative.
-
Hydrogen Sulfide (H₂S) Production: Negative.
-
Nitrate Reduction:
Positive (reduces nitrate to nitrite). -
Motility Test:
-
Y. pestis: Non-motile
-
Y. enterocolitica: Motile at 22–25°C, non-motile at 37°C
-
-
Phenylalanine Deaminase Test: Negative.
Pathogenicity
1. Yersinia pestis (Plague)
-
Disease Caused:
Plague – occurs in three clinical forms:-
Bubonic plague (most common)
-
Septicemic plague
-
Pneumonic plague (most severe and highly fatal)
-
-
Source & Transmission:
-
Natural reservoir: Rodents
-
Vector: Rat flea (Xenopsylla cheopis)
-
Pneumonic plague spreads by respiratory droplets.
-
-
Major Virulence Factors:
-
F1 capsular antigen: Anti-phagocytic protein capsule.
-
V and W antigens: Help survival inside macrophages.
-
Endotoxin (LPS): Causes fever, shock, and DIC.
-
Plasminogen activator: Facilitates spread in tissues.
-
Type III secretion system: Injects Yop proteins that inhibit phagocytosis.
-
-
Pathogenesis:
After entry, organisms multiply in lymph nodes causing painful swollen lymph nodes (buboes) → septicemia → dissemination to lungs and other organs.
2. Yersinia enterocolitica (Yersiniosis)
-
Disease Caused:
Yersiniosis, mainly affecting the gastrointestinal tract. -
Mode of Transmission:
-
Ingestion of contaminated food (pork, milk) or water.
-
Can grow at refrigerator temperature.
-
-
Clinical Manifestations:
-
Acute gastroenteritis (diarrhea, fever, abdominal pain)
-
Mesenteric lymphadenitis (mimics acute appendicitis)
-
Terminal ileitis
-
Post-infectious complications:
-
Reactive arthritis
-
Erythema nodosum
-
-
-
Virulence Factors:
-
Invasin protein: Facilitates entry into intestinal epithelial cells.
-
Yersinia outer proteins (Yops): Inhibit phagocytosis.
-
Heat-stable enterotoxin (Yst): Causes diarrhea.
-
Lipopolysaccharide (LPS): Endotoxic effects.
-
3. Yersinia pseudotuberculosis
Causes mesenteric lymphadenitis and ileitis, similar to Y. enterocolitica. Can produce scarlatiniform rash and systemic illness.
Laboratory Diagnosis
1. Specimen Collection
Yersinia pestis (Plague)
-
Bubonic plague:
Aspirate from bubo (lymph node) -
Septicemic plague:
Blood -
Pneumonic plague:
Sputum / throat swab
Yersinia enterocolitica
-
Stool sample (most common)
-
Blood (in septicemia)
-
Mesenteric lymph node biopsy (rare)
2. Microscopic Examination
-
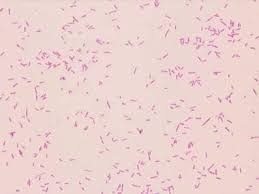
Gram Staining:
Shows Gram-negative, short plump bacilli. -
Special Staining:
-
Wayson / Giemsa / Leishman stain
-
Demonstrates bipolar (“safety-pin”) appearance, especially in Y. pestis.
-
3. Culture
Media Used
-
Blood agar:
Small, grayish, non-hemolytic colonies. -
MacConkey agar:
Non-lactose fermenting pale colonies. -
CIN agar (selective medium):
Especially for Y. enterocolitica – produces bull’s-eye colonies. -
Broth culture:
Y. pestis may show flocculent or stalactite growth.
Temperature
-
Optimal growth at 25–28°C.
-
Y. enterocolitica can be isolated by cold enrichment at 4°C.
4. Biochemical Identification
-
Oxidase: Negative
-
Catalase: Positive
-
Glucose: Fermented (acid only)
-
Urease:
-
Y. pestis – Negative
-
Y. enterocolitica – Positive
-
-
Indole:
-
Y. pestis – Negative
-
Y. enterocolitica – Positive
-
-
Motility:
-
Y. pestis – Non-motile
-
Y. enterocolitica – Motile at 22–25°C
-
5. Serological Tests
-
Antigen Detection:
Detection of F1 antigen of Y. pestis by:-
ELISA
-
Immunochromatographic tests
-
-
Antibody Detection:
Rising antibody titers in paired sera.
6. Molecular Methods
-
PCR:
Detection of specific genes for rapid and sensitive diagnosis, especially in plague outbreaks.
7. Animal Inoculation
-
Inoculation in guinea pig or mouse; animal dies rapidly in Y. pestis infection.
8. Safety Considerations
-
Y. pestis is a highly infectious organism.
-
Laboratory work must be done in biosafety level-3 (BSL-3) laboratories.
Antibiotic Resistance
1. General Features
-
Yersinia species show intrinsic resistance to certain antibiotics.
-
Resistance may be chromosomal or plasmid-mediated.
-
Antimicrobial susceptibility testing (AST) is recommended for all clinical isolates.
2. Intrinsic (Natural) Resistance
-
Penicillin G
-
First-generation cephalosporins
-
Ampicillin (common resistance due to β-lactamase production)
3. Acquired Resistance
-
Resistance genes may be carried on plasmids or transposons.
-
Increasing resistance reported to:
-
Tetracyclines
-
Chloramphenicol
-
Trimethoprim-sulfamethoxazole (in some strains)
-
-
Multidrug-resistant strains have been reported, especially in enteric Yersinia.
4. Species-Specific Resistance Patterns
Yersinia pestis
-
Generally susceptible to:
-
Streptomycin
-
Gentamicin
-
Doxycycline
-
Ciprofloxacin
-
-
Rare strains show resistance due to plasmid-mediated genes, especially in endemic regions.
Yersinia enterocolitica
-
Frequently resistant to:
-
Ampicillin
-
Amoxicillin
-
First-generation cephalosporins
-
-
Usually sensitive to:
-
Fluoroquinolones
-
Aminoglycosides
-
Third-generation cephalosporins
-
5. Mechanisms of Resistance
-
β-lactamase production → resistance to penicillins and early cephalosporins.
-
Efflux pumps → reduced intracellular antibiotic concentration.
-
Plasmid-encoded resistance genes → multidrug resistance.
-
Altered target sites → reduced drug binding.
6. Clinical & Public Health Importance
-
Empirical therapy should be based on local susceptibility patterns.
-
Emergence of resistant Y. pestis strains is a serious public health concern due to its potential for outbreaks.
-
Rational antibiotic use and surveillance are essential.
Prevention
1. Prevention of Plague (Yersinia pestis)
A. Reservoir and Vector Control
-
Rodent control in endemic areas.
-
Flea control using insecticides to prevent transmission.
-
Avoid handling dead rodents without protective measures.
B. Personal Protective Measures
-
Use of protective clothing and gloves when handling animals.
-
Respiratory protection (masks) for healthcare workers and close contacts in pneumonic plague.
C. Isolation and Surveillance
-
Isolation of suspected cases, especially pneumonic plague.
-
Active surveillance and early case detection in endemic regions.
-
Contact tracing and chemoprophylaxis for close contacts.
D. Chemoprophylaxis
-
Doxycycline or ciprofloxacin for close contacts of confirmed cases.
E. Vaccination
-
No widely available effective vaccine for general use.
-
Older killed vaccines are no longer recommended.
2. Prevention of Yersiniosis (Yersinia enterocolitica)
A. Food Safety Measures
-
Proper cooking of pork (common source).
-
Avoid consumption of unpasteurized milk and dairy products.
-
Wash fruits and vegetables thoroughly.
B. Water and Sanitation
-
Use safe drinking water.
-
Maintain proper hand hygiene, especially after handling raw meat.
C. Cold Storage Awareness
-
Y. enterocolitica can grow at refrigerator temperature → avoid prolonged storage of contaminated food.
D. Hospital Infection Control
-
Standard infection control precautions in healthcare settings.
-
Proper disinfection of contaminated surfaces and equipment.
3. General Preventive Measures
-
Health education in endemic and high-risk areas.
-
Early diagnosis and prompt treatment to prevent spread.
-
Reporting of cases to public health authorities.
MCQs
1. Yersinia belongs to which family?
A. Vibrionaceae
B. Pseudomonadaceae
C. Enterobacteriaceae
D. Neisseriaceae
Answer: C
2. Yersinia species are:
A. Gram-positive cocci
B. Gram-negative bacilli
C. Acid-fast bacilli
D. Spirochetes
Answer: B
3. The causative agent of plague is:
A. Yersinia enterocolitica
B. Yersinia pseudotuberculosis
C. Yersinia pestis
D. Yersinia ruckeri
Answer: C
4. The typical staining appearance of Yersinia pestis is:
A. Chain formation
B. Acid-fast rods
C. Bipolar (safety-pin) staining
D. Spiral shape
Answer: C
5. Which stain best demonstrates bipolar staining of Y. pestis?
A. Ziehl–Neelsen stain
B. Gram stain
C. Wayson stain
D. Albert stain
Answer: C
6. Yersinia species are:
A. Obligate aerobes
B. Obligate anaerobes
C. Facultative anaerobes
D. Microaerophilic
Answer: C
7. Which species is motile at 22–25°C but non-motile at 37°C?
A. Y. pestis
B. Y. enterocolitica
C. Y. pseudotuberculosis
D. All of the above
Answer: B
8. Yersinia pestis is:
A. Motile
B. Spore forming
C. Non-motile
D. Acid-fast
Answer: C
9. The capsule of Y. pestis is composed of:
A. Polysaccharide
B. Lipid
C. Protein (F1 antigen)
D. Peptidoglycan
Answer: C
10. The major vector for plague transmission is:
A. Mosquito
B. Louse
C. Tick
D. Rat flea
Answer: D
11. The flea involved in plague transmission is:
A. Ctenocephalides felis
B. Xenopsylla cheopis
C. Pediculus humanus
D. Anopheles
Answer: B
12. The most common form of plague is:
A. Pneumonic
B. Septicemic
C. Bubonic
D. Cutaneous
Answer: C
13. Painful swollen lymph nodes in plague are called:
A. Nodes
B. Buboes
C. Abscesses
D. Granulomas
Answer: B
14. Yersinia enterocolitica primarily causes:
A. Pneumonia
B. Gastroenteritis
C. Meningitis
D. Endocarditis
Answer: B
15. Y. enterocolitica infection may clinically mimic:
A. Typhoid fever
B. Appendicitis
C. Cholera
D. Dysentery
Answer: B
16. Yersinia enterocolitica commonly grows at:
A. Only 37°C
B. Only 42°C
C. Refrigerator temperature
D. Only anaerobic conditions
Answer: C
17. Selective medium for Y. enterocolitica is:
A. TCBS agar
B. Lowenstein–Jensen medium
C. CIN agar
D. Thayer–Martin agar
Answer: C
18. Colonies on CIN agar show:
A. Green colonies
B. Swarming
C. Bull’s-eye appearance
D. Metallic sheen
Answer: C
19. On MacConkey agar, Yersinia forms:
A. Lactose fermenting pink colonies
B. Non-lactose fermenting pale colonies
C. Mucoid colonies
D. Black colonies
Answer: B
20. Yersinia pestis shows which broth growth?
A. Uniform turbidity
B. Pellicle formation
C. Stalactite growth
D. No growth
Answer: C
21. Oxidase test of Yersinia is:
A. Positive
B. Weakly positive
C. Negative
D. Variable
Answer: C
22. Catalase reaction of Yersinia is:
A. Negative
B. Weakly positive
C. Positive
D. Variable
Answer: C
23. Urease test is positive in:
A. Y. pestis
B. Y. enterocolitica
C. Y. pestis and Y. pseudotuberculosis
D. All Yersinia species
Answer: B
24. Indole test is usually positive in:
A. Y. pestis
B. Y. enterocolitica
C. Y. pseudotuberculosis
D. None
Answer: B
25. Glucose fermentation by Yersinia produces:
A. Acid and gas
B. Gas only
C. Acid only
D. No fermentation
Answer: C
26. Major virulence factor inhibiting phagocytosis is:
A. Capsule
B. Flagella
C. Yops
D. Spores
Answer: C
27. Type III secretion system is characteristic of:
A. Yersinia
B. Vibrio
C. Neisseria
D. Streptococcus
Answer: A
28. Endotoxin of Yersinia is:
A. Exotoxin
B. Polysaccharide capsule
C. Lipopolysaccharide
D. Protein toxin
Answer: C
29. Specimen for suspected bubonic plague is:
A. Stool
B. Urine
C. Bubo aspirate
D. CSF
Answer: C
30. Safety-pin appearance is best seen in:
A. Culture media
B. Gram stain only
C. Special stains
D. Electron microscopy
Answer: C
31. Laboratory handling of Y. pestis requires:
A. BSL-1
B. BSL-2
C. BSL-3
D. BSL-4
Answer: C
32. Antibiotic of choice for plague is:
A. Penicillin
B. Streptomycin
C. Erythromycin
D. Vancomycin
Answer: B
33. Yersinia is naturally resistant to:
A. Aminoglycosides
B. Fluoroquinolones
C. Penicillin
D. Tetracycline
Answer: C
34. Common food source for Y. enterocolitica is:
A. Poultry
B. Beef
C. Pork
D. Fish
Answer: C
35. Post-infectious complication of yersiniosis includes:
A. Rheumatic fever
B. Reactive arthritis
C. Glomerulonephritis
D. Myocarditis
Answer: B
36. Which antigen is specific for Y. pestis?
A. O antigen
B. H antigen
C. F1 antigen
D. Vi antigen
Answer: C
37. Plague vaccine currently:
A. Widely used
B. Highly effective
C. Not routinely recommended
D. Mandatory
Answer: C
38. Cold enrichment technique helps in isolating:
A. Y. pestis
B. Y. enterocolitica
C. Salmonella
D. Shigella
Answer: B
39. Yersinia species are:
A. Strict human pathogens
B. Zoonotic organisms
C. Plant pathogens
D. Normal skin flora
Answer: B
40. Pneumonic plague spreads mainly by:
A. Flea bite
B. Fomites
C. Droplet infection
D. Food
Answer: C
41. Mesenteric lymphadenitis is commonly caused by:
A. Y. pestis
B. Y. enterocolitica
C. E. coli
D. Vibrio cholerae
Answer: B
42. Phenylalanine deaminase test in Yersinia is:
A. Positive
B. Negative
C. Variable
D. Weakly positive
Answer: B
43. H₂S production by Yersinia is:
A. Positive
B. Weak
C. Negative
D. Delayed
Answer: C
44. Reservoir of plague is mainly:
A. Humans
B. Birds
C. Rodents
D. Insects
Answer: C
45. The disease caused by Yersinia is called:
A. Yersinosis
B. Yersiniosis
C. Yersinitis
D. Yersinia fever
Answer: B
46. Bull’s-eye colonies are due to:
A. Capsule formation
B. Lactose fermentation
C. Mannitol fermentation on CIN agar
D. Hemolysis
Answer: C
47. Yersinia is non-lactose fermenter on:
A. Blood agar
B. Chocolate agar
C. MacConkey agar
D. TCBS agar
Answer: C
48. Endemic plague areas include:
A. Antarctica
B. Africa and Asia
C. Australia only
D. Europe only
Answer: B
49. Chemoprophylaxis for plague contacts includes:
A. Penicillin
B. Doxycycline
C. Vancomycin
D. Rifampicin
Answer: B
50. Most important virulence mechanism of Yersinia is:
A. Spore formation
B. Acid-fast cell wall
C. Inhibition of phagocytosis
D. Capsule polysaccharide only
Answer: C