Introduction
Cells are dynamic structures that constantly maintain internal balance (homeostasis). They adapt to stress through mechanisms such as hypertrophy, hyperplasia, atrophy, and metaplasia. However, when exposed to stress beyond their adaptive capacity, cellular injury occurs.
The severity and outcome of injury depend on: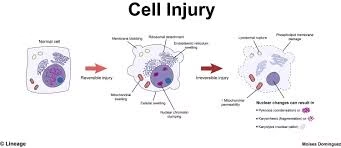
-
Nature of the injurious agent
-
Duration of exposure
-
Intensity of the insult
-
Type of cell affected
-
Nutritional and hormonal status
-
Genetic makeup of the individual
Cell injury progresses along a spectrum:
-
Adaptation → Reversible injury → Irreversible injury → Cell death
Causes of Cell Injury
Although causes are diverse, they can be grouped into major categories.
1. Hypoxia and Ischemia
Hypoxia is the most common cause of cell injury.
-
Hypoxia: Reduced oxygen availability
-
Ischemia: Reduced blood supply (oxygen + nutrients)
Common causes:
-
Myocardial infarction (coronary artery blockage)
-
Stroke (cerebral ischemia)
-
Severe anemia
-
Carbon monoxide poisoning
-
Shock
Oxygen is essential for oxidative phosphorylation in mitochondria. When oxygen supply decreases, ATP production falls, leading to energy failure.
2. Physical Agents
Physical injury may result from:
-
Mechanical trauma
-
Extreme heat (burns)
-
Extreme cold (frostbite)
-
Radiation exposure
-
Electric shock
-
Sudden pressure changes
Ionizing radiation damages cells by generating free radicals and causing DNA strand breaks.
3. Chemical Agents and Drugs
Many chemicals cause direct or indirect cellular damage.
Examples:
-
Industrial toxins
-
Pesticides
-
Heavy metals (lead, arsenic)
-
Alcohol
-
Chemotherapeutic drugs
Overdose of Paracetamol leads to accumulation of toxic metabolites that cause liver cell necrosis.
4. Infectious Agents
Microorganisms cause injury through toxin production, direct invasion, or immune-mediated mechanisms.
Examples:
-
Hepatitis B virus — causes liver cell injury
-
Mycobacterium tuberculosis — causes granulomatous inflammation
-
Fungal and parasitic infections
5. Immunologic Reactions
Immune responses may target self-tissues:
-
Autoimmune diseases
-
Hypersensitivity reactions
-
Chronic inflammatory disorders
Example: Autoimmune hepatitis causing hepatocyte injury.
6. Genetic Defects
Genetic mutations may lead to:
-
Abnormal enzyme function
-
Protein misfolding
-
Storage diseases
-
Metabolic imbalance
These defects predispose cells to injury even under normal conditions.
7. Nutritional Imbalance
-
Protein-energy malnutrition
-
Vitamin deficiencies
-
Obesity
-
Diabetes mellitus
Both deficiency and excess nutrients disturb metabolic processes.
Mechanisms of Cell Injury
Despite varied causes, most cell injuries follow common molecular pathways.
1. ATP Depletion
ATP is required for:
-
Sodium-potassium pump (Na⁺/K⁺ ATPase)
-
Protein synthesis
-
Lipid metabolism
-
Calcium transport
When ATP decreases:
-
Na⁺ accumulates inside cells
-
Water enters cells → swelling
-
Anaerobic glycolysis increases
-
Lactic acid accumulates
-
Intracellular pH decreases
Persistent ATP depletion leads to irreversible damage.
2. Mitochondrial Dysfunction
Mitochondria are the powerhouse of the cell.
Damage results in:
-
Reduced ATP production
-
Increased reactive oxygen species (ROS)
-
Release of pro-apoptotic proteins (e.g., cytochrome c)
Severe mitochondrial damage is a key event in irreversible injury.
3. Loss of Calcium Homeostasis
Normally, intracellular calcium levels are tightly regulated.
Injury causes calcium influx from:
-
Extracellular space
-
Endoplasmic reticulum
Elevated calcium activates:
-
Phospholipases → membrane damage
-
Proteases → cytoskeletal damage
-
Endonucleases → DNA fragmentation
-
ATPases → worsens ATP depletion
4. Oxidative Stress (Free Radical Injury)
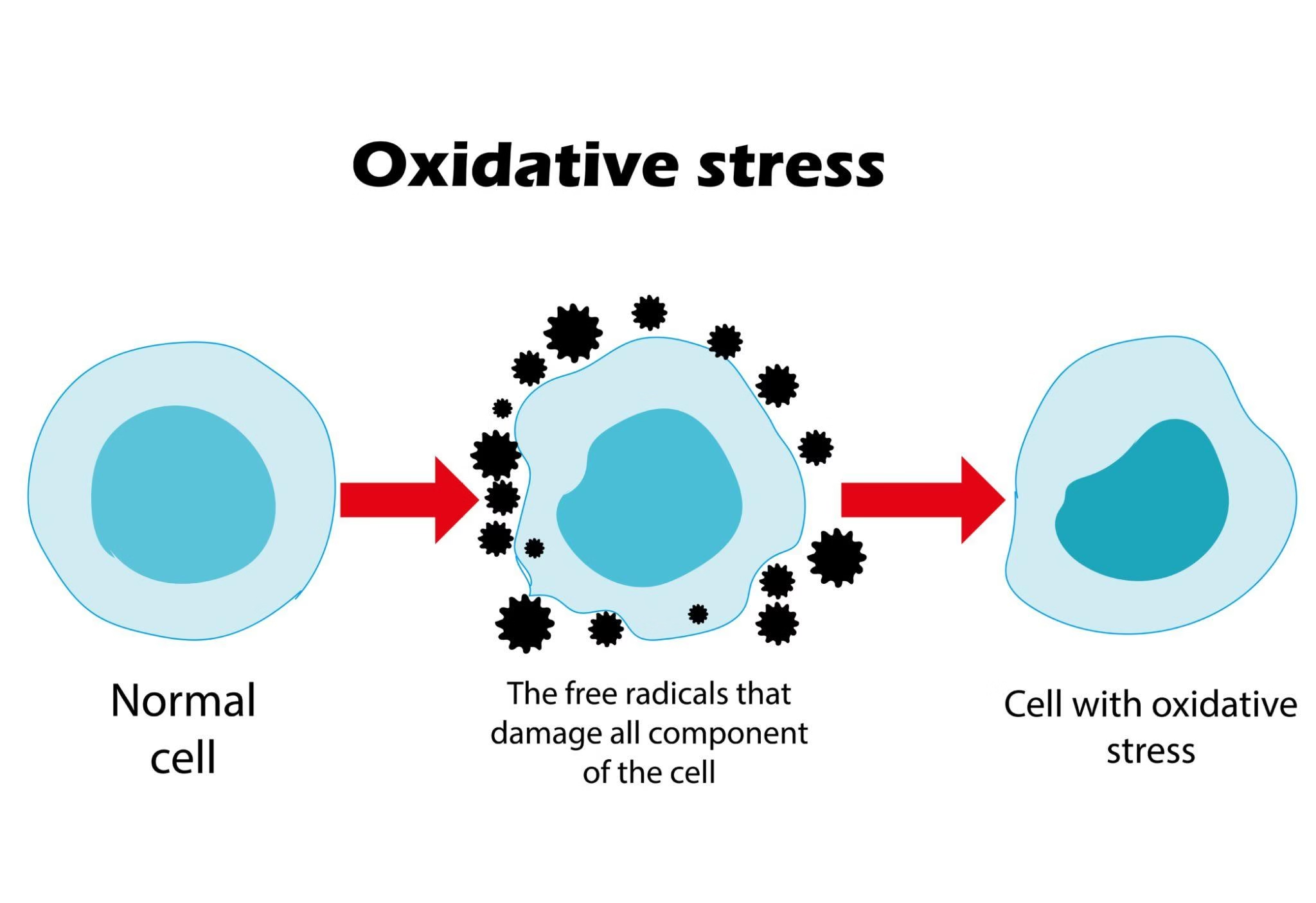
Free radicals contain unpaired electrons and are highly reactive.
Common ROS:
-
Superoxide (O₂⁻)
-
Hydrogen peroxide (H₂O₂)
-
Hydroxyl radical (OH⁻)
Effects:
-
Lipid peroxidation of membranes
-
Protein oxidation
-
DNA damage
Excessive ROS overwhelms antioxidant systems and leads to cell death.
5. Membrane Damage
Membrane integrity is essential for cell survival.
Damage may affect:
-
Plasma membrane
-
Mitochondrial membrane
-
Lysosomal membrane
Consequences:
-
Enzyme leakage
-
Calcium influx
-
Release of lysosomal enzymes
-
Autodigestion of cell
6. DNA and Protein Damage
Severe DNA injury activates p53-mediated pathways.
If repair fails:
-
Apoptosis is triggered
Protein misfolding leads to:
-
Endoplasmic reticulum stress
-
Activation of apoptosis
Reversible Cell Injury
Reversible injury occurs when:
-
The insult is mild
-
Exposure is short
-
The cause is removed early
Cells can recover completely.
Morphological Features

1. Cellular Swelling (Hydropic Change)
-
Most common early change
-
Due to failure of Na⁺/K⁺ pump
-
Cytoplasm appears pale and vacuolated
2. Fatty Change (Steatosis)
-
Common in liver and heart
-
Accumulation of triglycerides
-
Seen in alcohol-related liver disease
Ultrastructural Changes
-
Membrane blebbing
-
Mitochondrial swelling
-
Ribosomal detachment
-
Chromatin clumping
These changes are reversible if normal conditions are restored.
Irreversible Cell Injury
Irreversible injury leads to permanent damage and cell death.
Two principal forms:
-
Necrosis
-
Apoptosis
Hallmarks of Irreversible Injury
-
Severe mitochondrial dysfunction
-
Massive calcium influx
-
Extensive membrane damage
-
Lysosomal rupture
-
Nuclear destruction
Nuclear Changes
-
Pyknosis — nuclear shrinkage
-
Karyorrhexis — nuclear fragmentation
-
Karyolysis — dissolution of nucleus
These are diagnostic features of irreversible injury.
Necrosis
Necrosis is uncontrolled cell death caused by severe injury.
Characteristics:
-
Cell swelling
-
Plasma membrane rupture
-
Inflammation
-
Leakage of enzymes
Clinical example: Myocardial infarction causing cardiac muscle necrosis.
Types:
-
Coagulative necrosis
-
Liquefactive necrosis
-
Caseous necrosis
-
Fat necrosis
-
Fibrinoid necrosis
Apoptosis
Apoptosis is programmed cell death.
Features:
-
Cell shrinkage
-
Chromatin condensation
-
Formation of apoptotic bodies
-
No inflammation
Occurs in:
-
Embryogenesis
-
Hormone withdrawal
-
Mild DNA damage
Comparison: Reversible vs Irreversible Injury
| Feature | Reversible Injury | Irreversible Injury |
|---|---|---|
| ATP depletion | Mild/moderate | Severe |
| Membrane damage | Repairable | Irreparable |
| Nuclear changes | Minimal | Pyknosis, karyorrhexis |
| Outcome | Recovery | Cell death |
