Introduction
-
Infection prevention is a fundamental component of safe healthcare practice.
-
Hospitals and laboratories are high-risk environments for the spread of microorganisms.
-
Healthcare-associated infections (HAIs) increase patient morbidity, mortality, and healthcare costs.
-
Asepsis refers to the prevention of contamination by harmful microorganisms.
-
It includes practices designed to reduce or eliminate microbial presence.
-
Medical asepsis focuses on reducing the number and spread of microorganisms.
-
Surgical asepsis aims to eliminate all microorganisms, including spores.
-
Hand hygiene is the most effective and economical infection control measure.
-
Proper aseptic techniques help break the chain of infection.
-
These practices protect both patients and healthcare workers.
-
Strict adherence improves clinical outcomes and patient safety.

Asepsis
Asepsis refers to the absence of disease-causing microorganisms. It includes all practices that prevent contamination by pathogens and reduce the risk of infection.
Aseptic practices aim to:
-
Prevent introduction of pathogens into sterile body sites
-
Reduce microbial load in clinical settings
-
Protect healthcare workers and patients
-
Interrupt the chain of infection
Historical Background of Asepsis
-
Ignaz Semmelweis demonstrated that hand washing dramatically reduced maternal deaths due to puerperal fever.
-
Joseph Lister introduced antiseptic surgery using carbolic acid, reducing postoperative infections.
Their discoveries revolutionized infection control and laid the foundation of modern aseptic techniques.

Types of Asepsis
Asepsis is broadly classified into two types:
-
Medical Asepsis (Clean Technique)
-
Surgical Asepsis (Sterile Technique)
Both play distinct but complementary roles in infection prevention.
Medical Asepsis
Medical asepsis consists of practices that reduce the number and spread of microorganisms. It does not eliminate all microorganisms but minimizes their transmission.
Objectives
-
Prevent cross-contamination
-
Reduce microbial load
-
Control spread of infection within healthcare settings
Core Principles
-
Perform regular and proper hand hygiene
-
Use appropriate personal protective equipment (PPE)
-
Clean from least contaminated to most contaminated areas
-
Avoid shaking linens to prevent airborne spread
-
Dispose biomedical waste safely
-
Isolate infectious patients when necessary
Cleaning and Disinfection in Medical Asepsis
Cleaning
Cleaning is the physical removal of dirt, organic matter, and debris using water and detergents. It is the first and most essential step before disinfection or sterilization.
Disinfection
Disinfection destroys most pathogenic microorganisms, except bacterial spores.
Levels of Disinfection:
-
High-level disinfection (kills all microbes except spores)
-
Intermediate-level disinfection (kills mycobacteria, most viruses, bacteria)
-
Low-level disinfection (kills some bacteria and viruses)
Common hospital pathogens controlled through medical asepsis include:
-
Staphylococcus aureus
-
Escherichia coli
-
Pseudomonas aeruginosa
-
Klebsiella pneumoniae
Applications of Medical Asepsis
Medical asepsis is practiced in:
-
General ward care
-
Bed making and linen handling
-
Oral medication administration
-
Handling laboratory specimens
-
Cleaning patient surroundings
-
Dressing non-sterile wounds
-
Routine suctioning
Surgical Asepsis
Surgical asepsis involves procedures that eliminate all microorganisms, including bacterial spores. It is mandatory during invasive and surgical procedures.
Objectives
-
Prevent introduction of pathogens into sterile body cavities
-
Maintain sterility during procedures
-
Prevent surgical site infections (SSI)
Principles of Surgical Asepsis
-
Only sterile items should contact sterile items
-
Sterile field must remain in constant view
-
Items below waist level are considered contaminated
-
Moisture contaminates a sterile field
-
If sterility is in doubt, consider it contaminated
Sterilization Methods Used in Surgical Asepsis
-
121°C at 15 psi for 15–20 minutes
-
Destroys spores
-
Most reliable and commonly used method
2. Dry Heat Sterilization
-
160–170°C for 2 hours
-
Used for glassware, metal instruments
3. Gas Sterilization
-
Ethylene oxide
-
Suitable for heat-sensitive equipment
4. Radiation Sterilization
-
Gamma radiation for disposable medical supplies
Sterility Monitoring
-
Physical indicators (temperature, pressure monitoring)
-
Chemical indicators (color-changing strips)
-
Biological indicators (spore testing)
Hand Hygiene
Hand hygiene is the single most effective measure to prevent healthcare-associated infections.
According to the World Health Organization, proper hand hygiene significantly reduces infection transmission in healthcare settings.
Types of Hand Hygiene
1. Routine Hand Washing
-
Soap and water
-
40–60 seconds
-
Required when hands are visibly dirty
2. Alcohol-Based Hand Rub (ABHR)
-
20–30 seconds
-
Effective when hands are not visibly soiled
-
Rapid antimicrobial action
3. Surgical Hand Scrub
-
2–5 minutes
-
Includes hands and forearms
-
Performed before surgery
WHO’s Five Moments of Hand Hygiene
-
Before touching a patient
-
Before clean/aseptic procedures
-
After body fluid exposure
-
After touching a patient
-
After touching patient surroundings
Proper Hand Washing Technique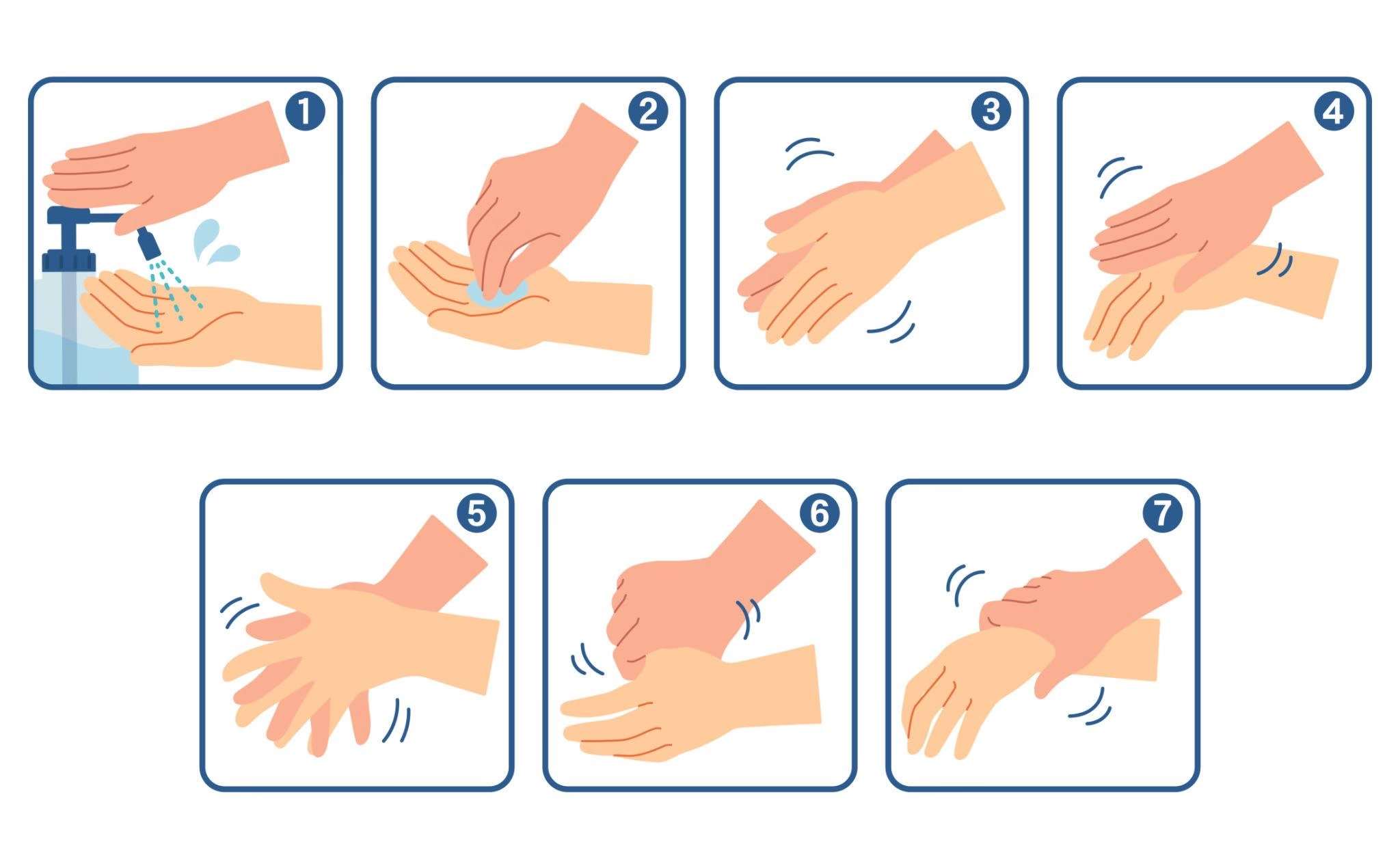
-
Wet hands with water
-
Apply soap
-
Rub palms together
-
Rub backs of hands
-
Interlace fingers
-
Clean thumbs
-
Clean fingertips and nails
-
Rinse thoroughly
-
Dry with clean towel
Duration: 40–60 seconds.
Importance of Hand Hygiene in Laboratory Practice
For Medical Laboratory Technologists (MLTs):
-
Perform hand hygiene before and after specimen handling
-
Use gloves appropriately
-
Avoid touching face during procedures
-
Decontaminate work surfaces
-
Follow biomedical waste protocols
Medical vs Surgical Asepsis: Key Differences
| Feature | Medical Asepsis | Surgical Asepsis |
|---|---|---|
| Objective | Reduce microorganisms | Eliminate all microorganisms |
| Also Known As | Clean technique | Sterile technique |
| Used In | Routine care | Invasive procedures |
| Sterility Required | No | Yes |
Consequences of Poor Aseptic Practices
Failure to follow aseptic principles may result in:
-
Surgical site infections
-
Bloodstream infections
-
Sepsis
-
Increased hospital stay
-
Antimicrobial resistance
-
Increased healthcare costs
