Introduction
-
Nosocomial infections, also known as hospital-acquired infections (HAIs), are infections that develop during a patient’s stay in a healthcare facility.
-
These infections are not present or incubating at the time of hospital admission.
-
They usually appear 48 hours or more after hospitalization, or within a few days after discharge.
-
Modern medical procedures such as surgeries, catheterization, mechanical ventilation, and invasive monitoring increase the risk of infection.
-
Prolonged hospital stay and use of broad-spectrum antibiotics further contribute to infection risk.
-
Nosocomial infections are a major global public health concern.
-
They increase patient morbidity, mortality, and healthcare costs.
-
High-risk groups include elderly patients, neonates, immunocompromised individuals, and ICU patients.
-
Common types include urinary tract infections, surgical site infections, ventilator-associated pneumonia, and bloodstream infections.
-
Frequently involved organisms include Staphylococcus aureus, Pseudomonas aeruginosa, and Klebsiella pneumoniae.
-
Prevention depends on strict infection control practices such as hand hygiene, aseptic techniques, sterilization, and antimicrobial stewardship.
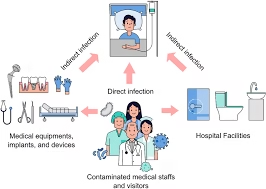
Definition of Nosocomial Infection
A nosocomial infection is defined as:
-
An infection that appears 48 hours or more after hospital admission,
-
Or within 3 days after discharge,
-
Or within 30 days after a surgical procedure (up to 1 year if an implant is placed),
-
And was not present or incubating at the time of admission.
These infections may affect patients, healthcare workers, and visitors.
Epidemiology
Nosocomial infections occur worldwide and affect both developed and developing countries. They are particularly common in:
-
Intensive Care Units (ICUs)
-
Surgical wards
-
Neonatal units
-
Burn units
-
Dialysis units
The incidence is higher in patients with:
-
Prolonged hospital stay
-
Immunosuppression
-
Invasive devices
-
Chronic diseases
The World Health Organization estimates that hundreds of millions of patients are affected globally each year, making HAIs a major public health problem.
Common Types of Nosocomial Infections
1. Urinary Tract Infections (UTIs)
-
Most common type of HAI
-
Often associated with urinary catheterization
-
Caused by organisms such as:
-
Escherichia coli
-
Klebsiella pneumoniae
-
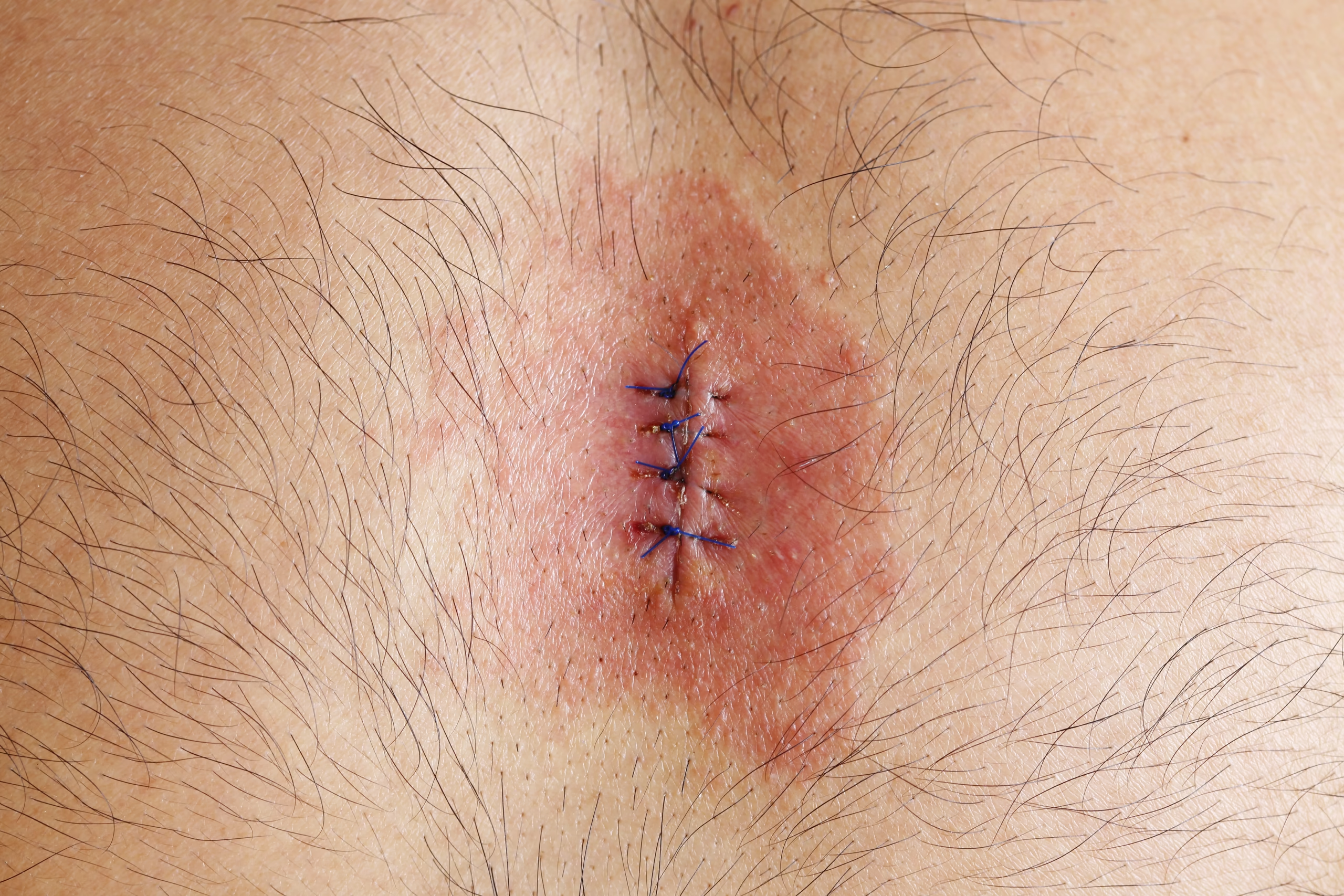
2. Surgical Site Infections (SSI)
-
Occur after surgical procedures
-
May involve skin, deep tissues, or organs
-
Common pathogens:
-
Staphylococcus aureus
-
Coagulase-negative staphylococci
-
3. Ventilator-Associated Pneumonia (VAP)
-
Occurs in patients on mechanical ventilation
-
Develops 48 hours after intubation
-
Common organisms:
-
Pseudomonas aeruginosa
-
Acinetobacter baumannii
-
4. Bloodstream Infections (BSI)
-
Associated with central venous catheters
-
May lead to sepsis
-
High mortality rate
Causative Microorganisms
Common Bacterial Agents:
-
Staphylococcus aureus
-
Escherichia coli
-
Klebsiella pneumoniae
-
Pseudomonas aeruginosa
-
Acinetobacter baumannii
Fungal Agents:
-
Candida species (especially in ICU patients)
Viral Agents:
-
Hepatitis B, Hepatitis C
-
Influenza virus
-
SARS-CoV-2
Many of these organisms show multidrug resistance (MDR), complicating treatment.
Sources of Nosocomial Infections
-
Endogenous sources (patient’s own flora)
-
Exogenous sources:
-
Healthcare workers’ hands
-
Contaminated instruments
-
Airborne droplets
-
Hospital surfaces
-
Improper sterilization
-
Risk Factors
Patient-Related Factors
-
Extremes of age
-
Immunosuppression
-
Diabetes mellitus
-
Malnutrition
-
Chronic illness
Hospital-Related Factors
-
Prolonged hospitalization
-
Invasive devices (catheters, ventilators)
-
Broad-spectrum antibiotic use
-
Poor hand hygiene compliance
-
Overcrowding
Mode of Transmission
Nosocomial infections spread through:
-
Direct contact
-
Indirect contact
-
Droplet transmission
-
Airborne transmission
-
Contaminated equipment
Breaking the chain of infection is crucial to prevention.
Diagnosis
Laboratory diagnosis plays a key role.
Steps include:
-
Proper specimen collection
-
Microscopy
-
Culture and sensitivity testing
-
Molecular methods (PCR)
-
Blood cultures for suspected sepsis
Medical laboratory technologists are essential in identifying pathogens and guiding antimicrobial therapy.
Prevention and Control Measures
1. Hand Hygiene
-
Most important preventive strategy
-
Alcohol-based hand rub
-
Proper hand washing technique
2. Sterilization and Disinfection
-
Autoclaving surgical instruments
-
High-level disinfection of endoscopes
-
Routine surface cleaning
3. Isolation Precautions
-
Contact precautions
-
Droplet precautions
-
Airborne precautions
4. Antimicrobial Stewardship
-
Rational antibiotic use
-
Avoid unnecessary broad-spectrum therapy
-
Monitor resistance patterns
5. Surveillance Programs
-
Continuous monitoring of infection rates
-
Reporting and analysis
-
Early outbreak detection
Role of Infection Control Committee (ICC)
Hospitals establish Infection Control Committees to:
-
Develop infection control policies
-
Monitor hospital infection rates
-
Conduct staff training
-
Implement outbreak control measures
-
Ensure compliance with guidelines
Complications of Nosocomial Infections
-
Sepsis
-
Septic shock
-
Organ failure
-
Prolonged hospital stay
-
Increased healthcare costs
-
Increased mortality
Economic Impact
Nosocomial infections:
-
Increase treatment expenses
-
Prolong ICU stays
-
Increase antibiotic consumption
-
Add financial burden to healthcare systems
Developing countries face greater challenges due to limited resources.
Emerging Challenges
-
Multidrug-resistant organisms (MDROs)
-
Carbapenem-resistant Enterobacteriaceae (CRE)
-
MRSA outbreaks
-
Increasing ICU admissions
-
Global pandemics
Antimicrobial resistance is one of the biggest threats to healthcare today.
